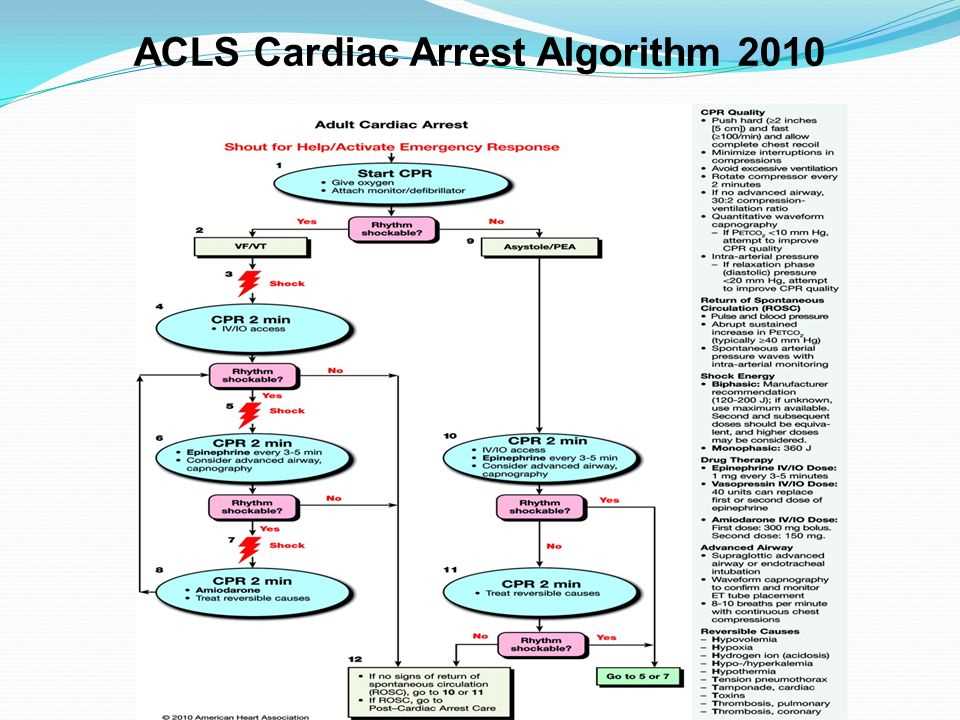
If you are preparing for the Advanced Cardiovascular Life Support (ACLS) certification exam in 2024, it is crucial to have a thorough understanding of the updated guidelines and be well-prepared with the correct answers. ACLS is a comprehensive course that equips healthcare providers with the knowledge and skills necessary to respond to cardiovascular emergencies. This article will provide you with the essential information and answers to common questions you may encounter in the ACLS exam to help you succeed.
One of the key areas to focus on for the ACLS exam is the management of cardiac arrest. This includes identifying the rhythm, performing high-quality CPR, and administering appropriate medications and defibrillation when needed. Understanding the algorithms and protocols for different cardiac arrest scenarios is essential, as the ACLS exam will test your ability to make timely and accurate decisions in these critical situations.
In addition to cardiac arrest management, the ACLS exam will also cover topics such as respiratory arrest, acute coronary syndromes, stroke, and post-cardiac arrest care. You should be familiar with the signs and symptoms of these conditions and understand the appropriate interventions and treatments. The exam may also assess your knowledge of airway management, pharmacology, and EKG interpretation.
To excel in the ACLS exam, it is recommended to thoroughly review the ACLS provider manual, attend hands-on practice sessions, and utilize online resources and practice exams. It is important to stay up-to-date with the most recent guidelines and be familiar with any updates or changes that may have been implemented since your last certification. By dedicating time and effort to your ACLS preparation, you will increase your chances of success and be better equipped to provide optimal care to patients in critical situations.
Acls Answers 2024
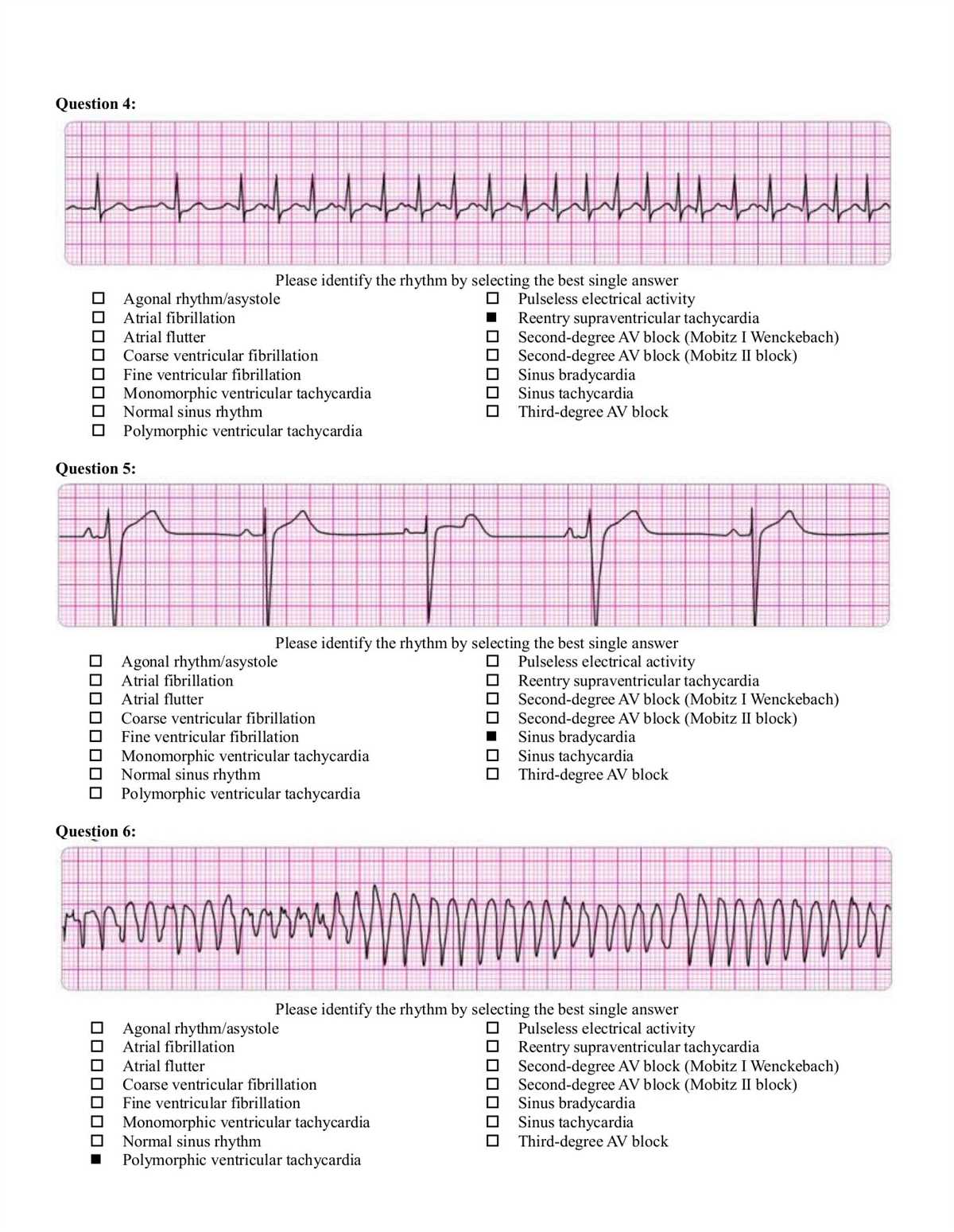
American Heart Association’s Advanced Cardiovascular Life Support (ACLS) is a crucial program designed to provide healthcare professionals with the knowledge and skills to effectively respond to cardiovascular emergencies. As medical guidelines and protocols are constantly updated, it is important for healthcare professionals to stay up-to-date with the latest information and practices. Here are some anticipated ACLS answers for the year 2024:
1. Enhanced Focus on Team-Based Approach
In 2024, ACLS training will continue to emphasize the importance of a team-based approach in addressing cardiovascular emergencies. Healthcare professionals will be educated on effective communication, leadership, and teamwork skills to ensure seamless coordination during critical situations. The training will also focus on improving interdisciplinary collaboration between different healthcare specialties, enabling better patient outcomes.
2. Integration of Simulation-Based Learning
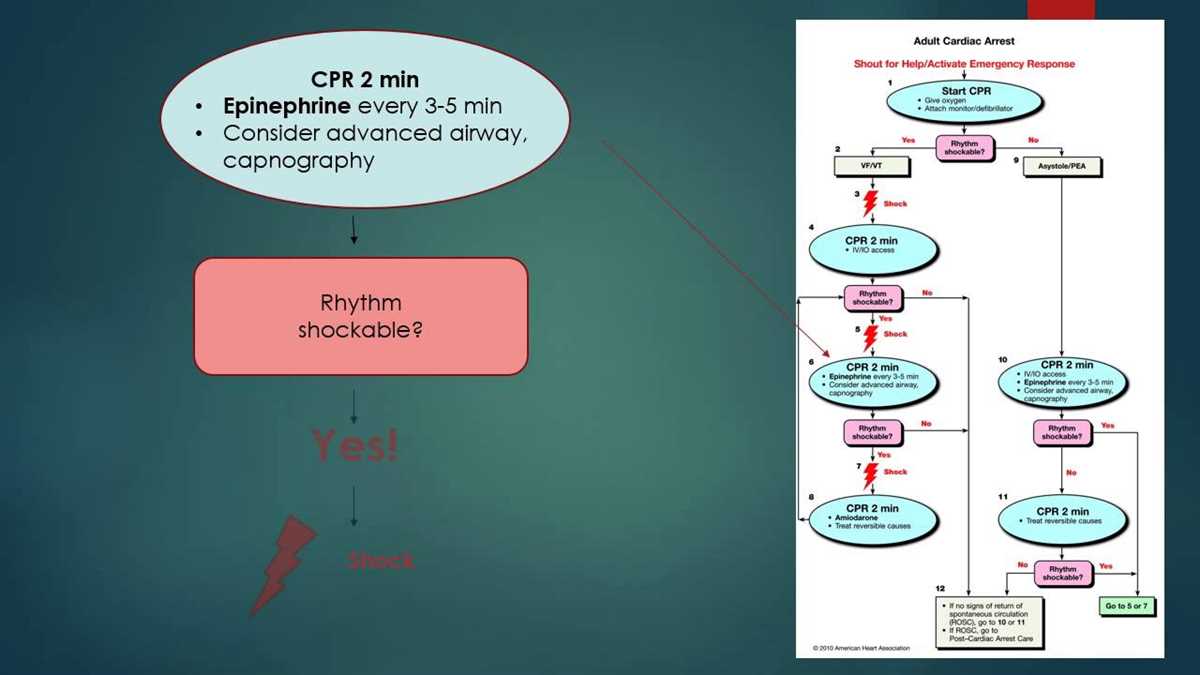
In the upcoming year, ACLS courses will increasingly incorporate simulation-based learning to enhance hands-on skills training. Simulated scenarios will allow healthcare professionals to practice their decision-making abilities and clinical interventions in a controlled environment. This approach will facilitate experiential learning, boost confidence, and help professionals better prepare for real-life situations where quick thinking and effective actions are required.
3. Updated Guidelines in Resuscitation and Medication Administration
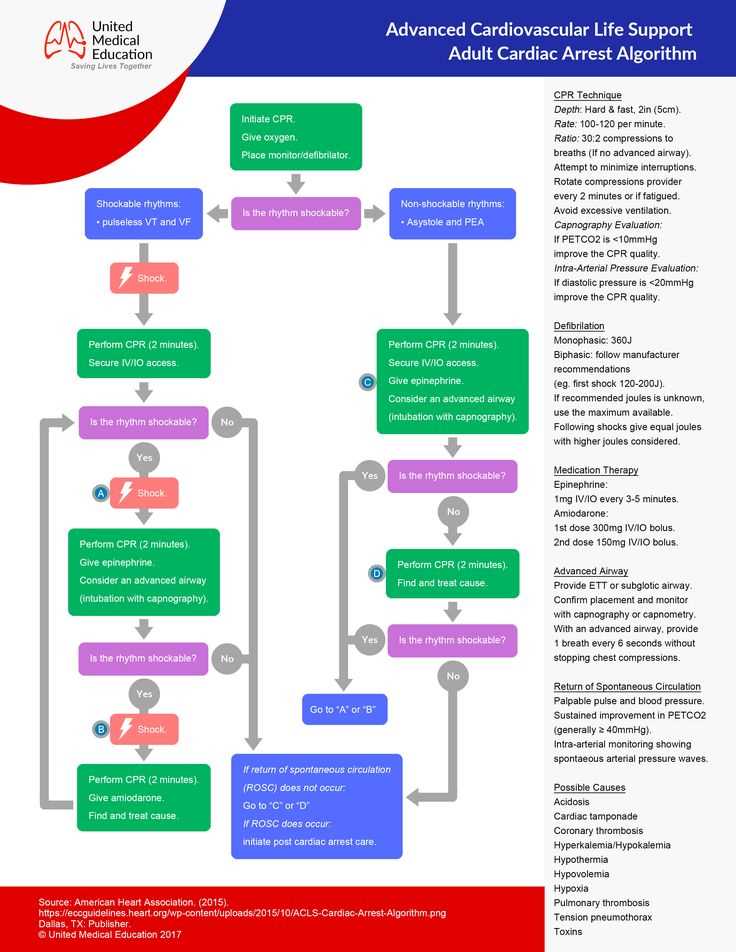
ACLS guidelines are reviewed and updated regularly to reflect the advancements in resuscitation science and evidence-based practices. In 2024, there will likely be updates in the recommended algorithms and approaches for CPR, defibrillation, and medication administration. Healthcare professionals will need to familiarize themselves with these updates to provide the most current and effective care to patients experiencing cardiac emergencies.
4. Expanded Focus on Post-Cardiac Arrest Care and Therapeutic Hypothermia
As research in post-cardiac arrest care and therapeutic hypothermia continues to evolve, ACLS courses in 2024 will place an increased emphasis on these areas. Healthcare professionals will receive updated information on the latest evidence-based strategies to improve neurological outcomes following resuscitation. This may include the use of targeted temperature management, neuroprotective strategies, and optimized post-resuscitation care protocols.
5. Integration of Technology and Data-driven Practices
In the digital age, the integration of technology and data-driven practices is becoming increasingly important in healthcare. In 2024, ACLS training may incorporate the use of technology such as point-of-care ultrasound (POCUS) and automated external defibrillators (AEDs) to improve diagnostic accuracy and optimize interventions. Additionally, healthcare professionals may be trained on utilizing electronic health records (EHRs) to access real-time patient information and make informed decisions during cardiovascular emergencies.
These anticipated ACLS answers for 2024 represent the potential developments and advancements in the field of resuscitation science and emergency cardiovascular care. Healthcare professionals should stay informed and engage in regular ACLS training to ensure their skills remain current and aligned with the latest guidelines and practices.
Overview of ACLS

Advanced Cardiovascular Life Support (ACLS) is a specialized training program that focuses on the management of cardiac arrest and other cardiovascular emergencies. It is designed for healthcare providers, such as doctors, nurses, and paramedics, who may be involved in the resuscitation and care of patients with life-threatening cardiac conditions.
The ACLS certification course covers a wide range of topics, including the recognition and treatment of various cardiac dysrhythmias, the use of advanced life support equipment such as defibrillators and cardiac monitors, and the administration of medications to manage cardiac emergencies. It also emphasizes the importance of effective teamwork and communication during resuscitation efforts.
The ACLS algorithms provide step-by-step protocols to guide healthcare providers in the management of specific cardiac conditions. These algorithms cover a variety of scenarios, including cardiac arrest, bradycardia, tachycardia, and pulseless electrical activity. They provide a systematic approach to assessment, treatment, and ongoing monitoring of patients with critical cardiac conditions.
ACLS certification is typically valid for two years, and healthcare providers are required to renew their certification regularly to maintain their knowledge and skills in emergency cardiovascular care. ACLS training is often a required component of many healthcare professions, and individuals who complete the course may have enhanced career opportunities and the ability to respond effectively to cardiac emergencies in various settings.
The Importance of ACLS Certification

ACLS (Advanced Cardiovascular Life Support) certification is a critical accreditation for healthcare professionals working in emergency settings, such as hospitals, clinics, and paramedic services. This certification equips healthcare providers with the necessary knowledge and skills to effectively respond to cardiovascular emergencies and save lives. It is a recognized standard for providing evidence-based treatment algorithms and techniques for managing cardiac arrest, stroke, and other life-threatening conditions.
One of the key benefits of ACLS certification is the ability to enhance patient outcomes. By obtaining this certification, healthcare professionals gain a comprehensive understanding of the latest advancements in resuscitation procedures and emergency cardiovascular care. This allows them to make informed decisions during high-pressure situations, leading to improved patient survival rates and reduced morbidity.
- Increased Competency: ACLS certification ensures that healthcare providers have a solid understanding of advanced cardiac life support techniques, including airway management, defibrillation, and medication administration. This competency enables them to take immediate action when faced with critical situations, increasing the chances of a positive patient outcome.
- Teamwork and Collaboration: ACLS training emphasizes the importance of effective teamwork and communication during emergency situations. Healthcare professionals with ACLS certification learn how to work together seamlessly, ensuring optimal patient care and reducing the risk of errors.
- Professional Development: ACLS certification is often a requirement for healthcare professionals seeking career advancement in critical care and emergency medicine. By obtaining this certification, individuals enhance their professional credentials and open up new opportunities for career growth.
In conclusion, ACLS certification plays a vital role in ensuring the delivery of high-quality emergency cardiovascular care. It equips healthcare professionals with the necessary skills and knowledge to respond effectively to life-threatening situations, leading to improved patient outcomes and increased career prospects in the field of critical care. It is an essential accreditation for any healthcare professional working in an emergency setting.
Changes in ACLS Guidelines for 2024
The American Heart Association (AHA) has recently released the updated Advanced Cardiovascular Life Support (ACLS) guidelines for 2024. These guidelines aim to provide healthcare professionals with the most current, evidence-based recommendations for the management of cardiac arrest and other cardiovascular emergencies.
One significant change in the ACLS guidelines for 2024 is the emphasis on high-quality, uninterrupted chest compressions during cardiopulmonary resuscitation (CPR). The guidelines now recommend a compression-only CPR approach for bystanders who witness a sudden cardiac arrest. This simplification of CPR protocols is intended to empower bystanders and increase the likelihood of early intervention, ultimately improving survival rates.
Another important update in the ACLS guidelines is the inclusion of targeted temperature management for post-cardiac arrest care. The guidelines now recommend maintaining a targeted temperature between 32°C and 36°C for at least 24 hours in adult patients who remain comatose after successful resuscitation. This approach has been shown to improve neurological outcomes and survival rates in patients who experience cardiac arrest.
In addition, the ACLS guidelines for 2024 place increased emphasis on the use of mechanical CPR devices during prolonged resuscitation efforts. These devices, such as load-distributing band CPR (LDB-CPR) and piston-driven devices, can provide consistent and high-quality chest compressions, allowing healthcare providers to focus on other aspects of patient care during resuscitation efforts.
Overall, the updated ACLS guidelines for 2024 reflect advances in resuscitation science and clinical research, with a focus on simplifying protocols, improving outcomes, and providing the most effective care for patients experiencing cardiac arrest. Healthcare professionals should familiarize themselves with these changes to ensure they are delivering the highest level of care to their patients.
Key Points to Remember in ACLS
Advanced Cardiovascular Life Support (ACLS) is a set of clinical interventions and algorithms designed to provide resuscitation and stabilization to patients experiencing cardiac arrest or other life-threatening emergencies. It is important for healthcare professionals to understand and remember key points in ACLS to effectively respond to these critical situations.
1. Basic life support (BLS) is the foundation: Before initiating ACLS interventions, providers must ensure that basic life support measures, such as chest compressions and ventilation, are being performed effectively. Proper BLS techniques form the foundation of ACLS care.
2. Rapid recognition and intervention: Time is critical in ACLS, and providers must be able to rapidly recognize the signs of cardiac arrest and initiate appropriate interventions. Early defibrillation, administration of medications, and advanced airway management are examples of interventions that can improve patient outcomes.
- Early defibrillation: Delivering a shock to the heart as soon as possible can help restore a normal heart rhythm.
- Medication administration: ACLS protocols include specific medications, such as epinephrine and amiodarone, which may be needed to restore circulation and maintain a stable cardiac rhythm.
- Advanced airway management: In some cases, advanced airway techniques, such as endotracheal intubation or supraglottic airway placement, may be necessary to ensure adequate oxygenation and ventilation.
3. Continuous monitoring and reassessment: Throughout the ACLS resuscitation process, providers must continuously monitor the patient’s vital signs, cardiac rhythm, and response to interventions. Regular reassessment allows for adjustments in care and identification of potential complications.
4. Effective team dynamics: Successful ACLS care relies on effective teamwork and communication. Providers must be able to work collaboratively, assign roles, and communicate clearly in order to provide seamless and coordinated care to the patient.
In summary, ACLS requires a thorough understanding of key points, including the importance of basic life support, rapid recognition and intervention, continuous monitoring and reassessment, and effective team dynamics. By following these principles, healthcare professionals can improve patient outcomes in cardiac emergencies.
Common ACLS Scenarios and Their Answers
ACLS (Advanced Cardiovascular Life Support) scenarios are designed to test healthcare professionals’ ability to respond to critical cardiac emergencies. These scenarios often require quick thinking, appropriate assessment, and effective intervention. Understanding the common scenarios that can occur during ACLS can help healthcare providers prepare and respond appropriately.
One of the common scenarios in ACLS is cardiac arrest. In this scenario, the primary goal is to initiate high-quality CPR (cardiopulmonary resuscitation) immediately while activating the emergency response system. Healthcare providers should assess for the presence of a shockable rhythm (ventricular fibrillation or pulseless ventricular tachycardia) and deliver defibrillation as soon as possible. If the rhythm is not shockable, providers should continue high-quality CPR, administer appropriate medications, and consider advanced airway management.
Scenario: A patient presents with symptoms of acute coronary syndrome and is diagnosed with ST-segment elevation myocardial infarction (STEMI).
For this scenario, the primary goal is to provide reperfusion therapy as quickly as possible. Healthcare providers should administer aspirin and initiate intravenous access. If the patient meets the criteria for percutaneous coronary intervention (PCI), the patient should be transferred immediately to the cardiac catheterization lab. If PCI is not available within a timely manner, fibrinolytic therapy should be considered.
Scenario: A patient with known atrial fibrillation presents with rapid ventricular response and signs of hemodynamic instability.
In this scenario, the primary goal is to control the ventricular rate and stabilize the patient’s hemodynamics. Healthcare providers should administer intravenous medications such as beta-blockers, calcium channel blockers, or amiodarone to slow the ventricular rate. If the patient remains unstable despite medical therapy, synchronized cardioversion may be necessary.
Scenario: A patient presents with signs and symptoms of acute ischemic stroke.
The primary goal in this scenario is to expedite evaluation and treatment to minimize neurological damage. Healthcare providers should assess the patient’s eligibility for thrombolytic therapy within the appropriate time window. If eligible, intravenous alteplase should be administered. Additionally, a stroke code should be activated, and the patient should undergo further evaluation, including neuroimaging.
Scenario: A patient presents with symptomatic bradycardia and signs of inadequate perfusion.
In this scenario, the primary goal is to improve perfusion and stabilize the patient’s condition. Healthcare providers should assess for reversible causes and intervene appropriately, such as administering atropine or initiating transcutaneous pacing. If these measures are ineffective, the provider may consider administering chronotropic agents or transvenous pacing.