Subjective data is an essential part of any focused exam, including the assessment of abdominal pain. Shadow health focused exam abdominal pain subjective data helps healthcare providers gain a comprehensive understanding of the patient’s symptoms, medical history, and other relevant information. This type of data is gathered directly from the patient and includes their perception of the pain, its location, severity, duration, associated symptoms, and any potential aggravating or alleviating factors.
When assessing a patient with abdominal pain, it is crucial to inquire about the onset and progression of the pain, as well as any factors that may have triggered it. Patients may describe their pain as sudden or gradual, constant or intermittent, mild or severe. They may also mention any changes in the pain over time, such as worsening or improvement.
In addition to pain characteristics, healthcare providers should ask about other symptoms that the patient may be experiencing. These may include nausea, vomiting, diarrhea, constipation, bloating, gas, fever, chills, fatigue, weight loss, loss of appetite, urinary symptoms, or any other associated discomfort. The presence of these symptoms can provide insights into the possible underlying cause of the abdominal pain and can help guide further examination and diagnostic tests.
Understanding Shadow Health Focused Exam: Abdominal Pain Subjective Data
During a Shadow Health Focused Exam on abdominal pain, the subjective data collection is a crucial step in understanding the patient’s symptoms, history, and overall condition. By gathering information directly from the patient, healthcare providers can gain valuable insights and develop a targeted care plan.
When conducting the subjective data collection, it is essential to ask open-ended questions to allow the patient to provide detailed information about their abdominal pain. Questions like “Can you describe the location and intensity of your pain?” and “How long have you been experiencing these symptoms?” can help identify the possible causes and severity of the condition.
Additionally, it is important to ask about any factors that worsen or alleviate the pain, such as certain movements, eating, or medication. This information can help in pinpointing the underlying cause and identifying potential triggers or treatment options for the patient.
Furthermore, inquiring about the patient’s medical history, including any previous abdominal surgeries, gastrointestinal conditions, or family history of abdominal problems, can provide valuable context and help in formulating a comprehensive care plan.
Focusing on the patient’s overall health and lifestyle is also crucial. Inquiring about their diet, exercise routines, stress levels, and any recent life changes can help identify potential contributing factors to their abdominal pain. Additionally, assessing the patient’s mental health and emotional well-being can provide insights into the overall impact of their condition on their daily life.
Gathering comprehensive subjective data during a Shadow Health Focused Exam for abdominal pain is essential for accurate diagnosis and effective treatment planning. By eliciting detailed information from the patient, healthcare providers can offer personalized care and improve patient outcomes.
What is a Shadow Health Focused Exam?
A Shadow Health Focused Exam is an interactive and virtual patient encounter that allows healthcare providers and students to practice and develop their clinical skills. It simulates a real-life patient examination, providing an opportunity to gather subjective and objective data, make clinical judgments, and create a care plan.
During a Shadow Health Focused Exam, learners engage with a virtual patient through an online platform. They can ask the patient questions, perform physical assessments, and document their findings in a structured manner. The virtual patient responds to the learner’s actions and inquiries, providing realistic and dynamic interactions.
The use of Shadow Health Focused Exams offers several benefits to healthcare practitioners and students. It allows for practice in a safe and controlled environment, where mistakes can be made without harm to real patients. It also provides immediate feedback, allowing learners to reflect on their actions and improve their skills. Additionally, Shadow Health Focused Exams can be accessed anytime and anywhere, providing flexibility for learning and assessment.
In conclusion, a Shadow Health Focused Exam is a valuable tool for healthcare providers and students to develop their clinical competency. It offers a realistic and immersive virtual patient encounter, enabling learners to practice and refine their patient examination skills, critical thinking, and clinical decision-making abilities.
Overview of Abdominal Pain
Abdominal pain refers to any discomfort or pain felt in the area between the chest and the pelvis. It can vary in intensity and duration, and can be caused by a wide range of underlying conditions. Abdominal pain can be classified as acute or chronic, depending on the duration of the pain. Acute abdominal pain typically presents suddenly and may be severe. Chronic abdominal pain, on the other hand, persists for a longer period of time, often lasting for weeks or months.
There are several possible causes of abdominal pain, including gastrointestinal issues, such as gastroenteritis, gastritis, peptic ulcers, and irritable bowel syndrome. Other potential causes include urinary tract infections, kidney stones, appendicitis, hernias, and ovarian cysts. In some cases, abdominal pain may also be a symptom of more serious conditions, such as pancreatitis, gallstones, or an abdominal aortic aneurysm.
When evaluating a patient with abdominal pain, it is important to obtain a detailed medical history and perform a physical examination. The location, quality, and severity of the pain can provide valuable clues as to the underlying cause. Additional diagnostic tests, such as blood work, imaging studies (such as ultrasound or CT scan), and endoscopy, may be necessary to further evaluate the source of the pain. Treatment for abdominal pain will depend on the underlying cause, and may include medication, lifestyle changes, or in some cases, surgical intervention.
Importance of Collecting Subjective Data
Collecting subjective data is an essential step in evaluating a patient’s health status, particularly when assessing symptoms such as abdominal pain. Subjective data provides valuable insights into the patient’s experience, perception, and interpretation of their symptoms, allowing healthcare providers to gather critical information about the possible causes and potential diagnoses. It helps establish trust between the healthcare provider and the patient, as it demonstrates that the provider is interested in understanding the patient’s individual experience and tailoring the care accordingly.
Subjective data is often obtained through open-ended questions, allowing patients to freely express their concerns and describe their symptoms in their own words. This enables healthcare providers to gather a comprehensive understanding of the patient’s symptoms, including the location, quality, severity, and aggravating or alleviating factors. Through active listening and effective communication, healthcare providers can further explore the patient’s medical history, family history, lifestyle factors, and any recent changes that may be contributing to the abdominal pain.
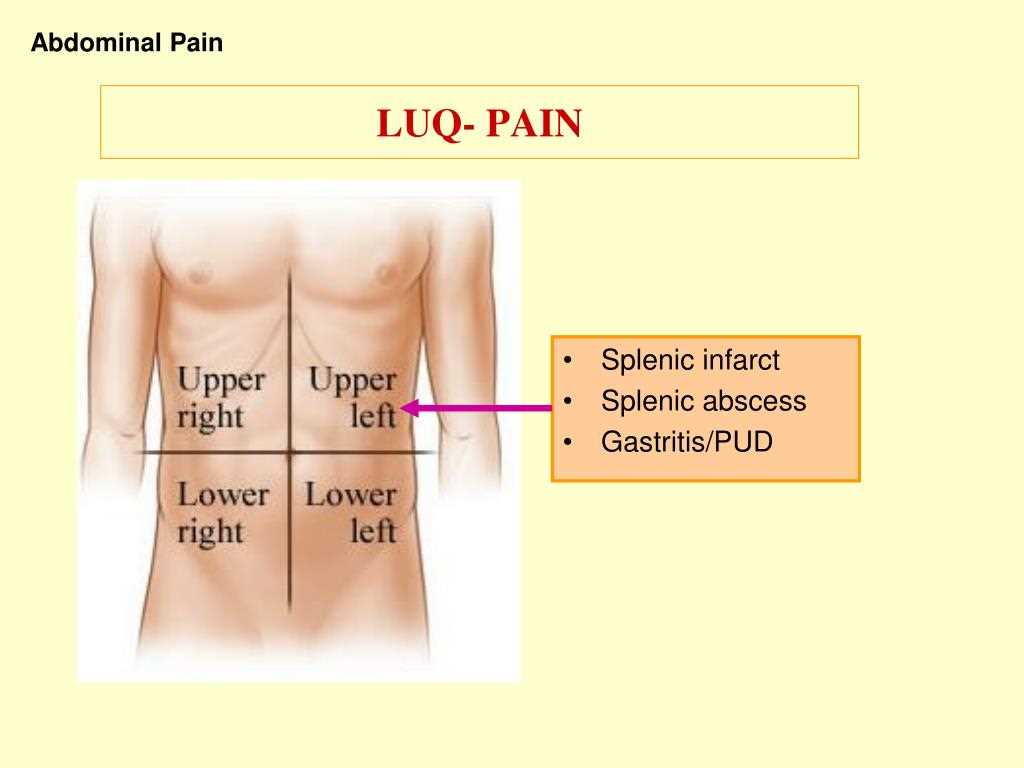
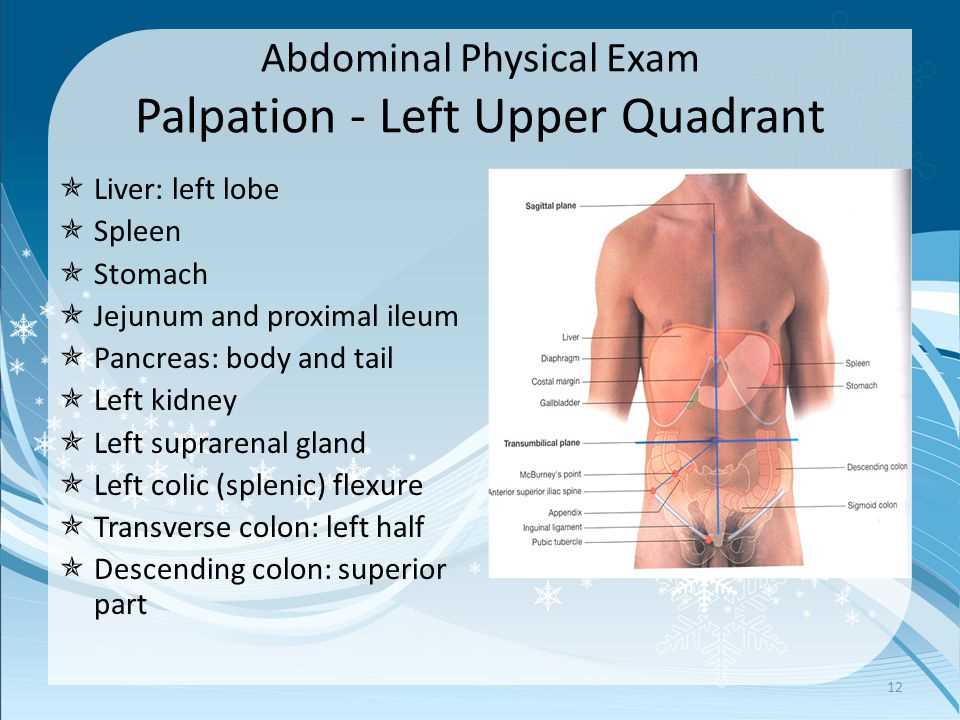
- Location: Asking the patient to pinpoint the exact location of the abdominal pain can help healthcare providers identify potential underlying causes. Different areas of the abdomen may be associated with different organs or systems, such as upper abdominal pain suggesting gastric or liver issues, or lower abdominal pain indicating potential gastrointestinal or reproductive problems.
- Quality: Understanding the quality of the pain, such as sharp, dull, cramp-like, or burning, can provide further clues about potential causes. For example, sharp stabbing pain may indicate a gastrointestinal issue, while cramp-like pain could suggest menstrual or digestive problems.
- Severity: Assessing the severity of the pain can help determine the urgency of the situation and guide appropriate interventions. Using pain scales or asking patients to rate their pain on a scale of 1 to 10 can provide valuable information for healthcare providers.
- Aggravating/Alleviating factors: Identifying factors that worsen or relieve the pain, such as movement, eating, or specific positions, can help healthcare providers narrow down potential causes and develop appropriate management strategies.
In conclusion, subjective data is crucial in accurately assessing abdominal pain and other symptoms. It enables healthcare providers to gather essential information about the patient’s experience, helping them formulate appropriate diagnoses and treatment plans. By actively listening and asking relevant questions, healthcare providers can build a trusting relationship with the patient, fostering effective communication and improved patient outcomes.
Key Components of the Shadow Health Focused Exam: Abdominal Pain Subjective Data
When conducting a focused exam on a patient with abdominal pain, there are several key components that should be addressed in the subjective data collection. These components include gathering information about the nature of the pain, its location and radiation, its onset and duration, aggravating and alleviating factors, associated symptoms, and the patient’s medical history.
The nature of the pain: It is important to ask the patient about the characteristics of the pain. Is it sharp, dull, cramping, or burning? Does it come and go or is it constant? This information can provide valuable insights into the possible causes of the pain.
Location and radiation: Determining where the pain is located and whether it radiates to other areas can help narrow down possible causes. For example, pain in the right lower quadrant may suggest appendicitis, while pain that radiates to the back may indicate a pancreatic issue.
Onset and duration: Understanding when the pain first started and how long it has been present can assist in determining the urgency of further evaluation and investigation. A sudden onset of severe pain may indicate an acute condition, while chronic or intermittent pain may point to a more long-standing issue.
Aggravating and alleviating factors: Inquiring about activities or positions that worsen or relieve the pain can provide clues as to its cause. For example, does eating aggravate the pain, or does lying down alleviate it?
Associated symptoms: It is important to inquire about any accompanying symptoms that the patient may be experiencing. These can include nausea, vomiting, changes in bowel movements, fever, or weight loss. These symptoms can help further narrow down the possible causes of the abdominal pain.
Medical history: Gathering information about the patient’s medical history, including any previous abdominal surgeries, chronic conditions, or medications, is crucial in evaluating the possible causes of the pain. Certain conditions or medications may predispose patients to specific abdominal issues.
By thoroughly assessing these key components of the subjective data, healthcare providers can gather the necessary information to develop a focused plan for further evaluation, testing, and treatment of the patient’s abdominal pain.
Tips for Conducting an Effective Interview
Interviewing patients is a crucial part of obtaining subjective data and understanding their health concerns. Here are some tips for conducting an effective interview:
- Establish rapport: Begin the interview by introducing yourself and building a rapport with the patient. Show empathy, active listening, and maintain a non-judgmental attitude to gain the patient’s trust.
- Prepare and be organized: Prior to the interview, review the patient’s medical history, relevant lab results, and any available notes. Have a structured plan and ensure all necessary tools and documents are ready.
- Use open-ended questions: Encourage patients to provide detailed information by asking open-ended questions such as “Tell me more about…”. Avoid leading questions that may bias the patient’s responses.
- Active listening: Give your full attention to the patient and maintain good eye contact. Listen attentively to the patient’s responses, avoid interrupting, and use reflective responses to show that you understand and validate their concerns.
- Respect cultural differences: Be mindful of cultural differences that may affect the patient’s views on health, illness, and healthcare. Respect their beliefs and communication styles, and adapt your approach accordingly.
- Use appropriate language: Ensure that your language is clear, simple, and jargon-free. Avoid medical jargon and explain any terms or concepts that might be unfamiliar to the patient.
- Non-verbal communication: Pay attention to your own non-verbal cues, such as body language, facial expressions, and tone of voice. Be aware of the patient’s non-verbal cues as well, as they can provide valuable insights into their emotions and concerns.
- Maintain confidentiality: Assure the patient that their information will be kept confidential and that their privacy will be respected. Maintain appropriate documentation practices and follow HIPAA guidelines.
By following these tips, healthcare providers can conduct effective interviews that allow them to gather accurate and comprehensive subjective data from their patients. This information is essential for making accurate diagnoses, developing appropriate treatment plans, and providing high-quality patient care.
Q&A:
What are some tips for conducting an effective interview?
When conducting an interview, it is important to thoroughly prepare beforehand. Research the candidate’s background and come up with a list of relevant questions. During the interview, actively listen to the candidate’s responses and ask follow-up questions to gather more information. It is also important to create a comfortable and welcoming environment for the candidate, as this can help them open up and provide more insightful answers. Finally, make sure to take detailed notes during the interview and evaluate each candidate objectively based on their qualifications and fit for the position.
How can I make sure I ask the right questions during an interview?
To ask the right questions during an interview, start by reviewing the job description and identifying the key skills and qualifications required for the position. Tailor your questions to assess these specific areas. Try to ask open-ended questions that require the candidate to provide detailed responses, rather than simple yes or no answers. Ask behavioral questions that require the candidate to provide real-life examples of their skills and experiences. Finally, don’t forget to ask about the candidate’s future goals and how they align with the company’s mission and values.
How can I create a comfortable environment for the candidate during an interview?
Creating a comfortable environment for the candidate during an interview is crucial to encourage open and honest communication. Start by greeting the candidate warmly and introducing yourself and the interview process. Offer the candidate a glass of water and ensure the interview room is clean and well-lit. Make eye contact, smile, and use positive body language to make the candidate feel at ease. Be an active listener and show genuine interest in the candidate’s responses. Avoid interrupting or being overly critical, and give the candidate enough time to think and respond to each question.
What should I do after conducting an interview?
After conducting an interview, it is important to take some time to evaluate each candidate objectively. Review your notes, compare each candidate’s qualifications and fit for the position, and make a list of the pros and cons for each candidate. Consider both their technical skills and their cultural fit within the company. If necessary, consult with relevant team members or superiors to gather additional feedback. Finally, contact the successful candidate to offer them the job and provide feedback to the other candidates in a respectful and professional manner.