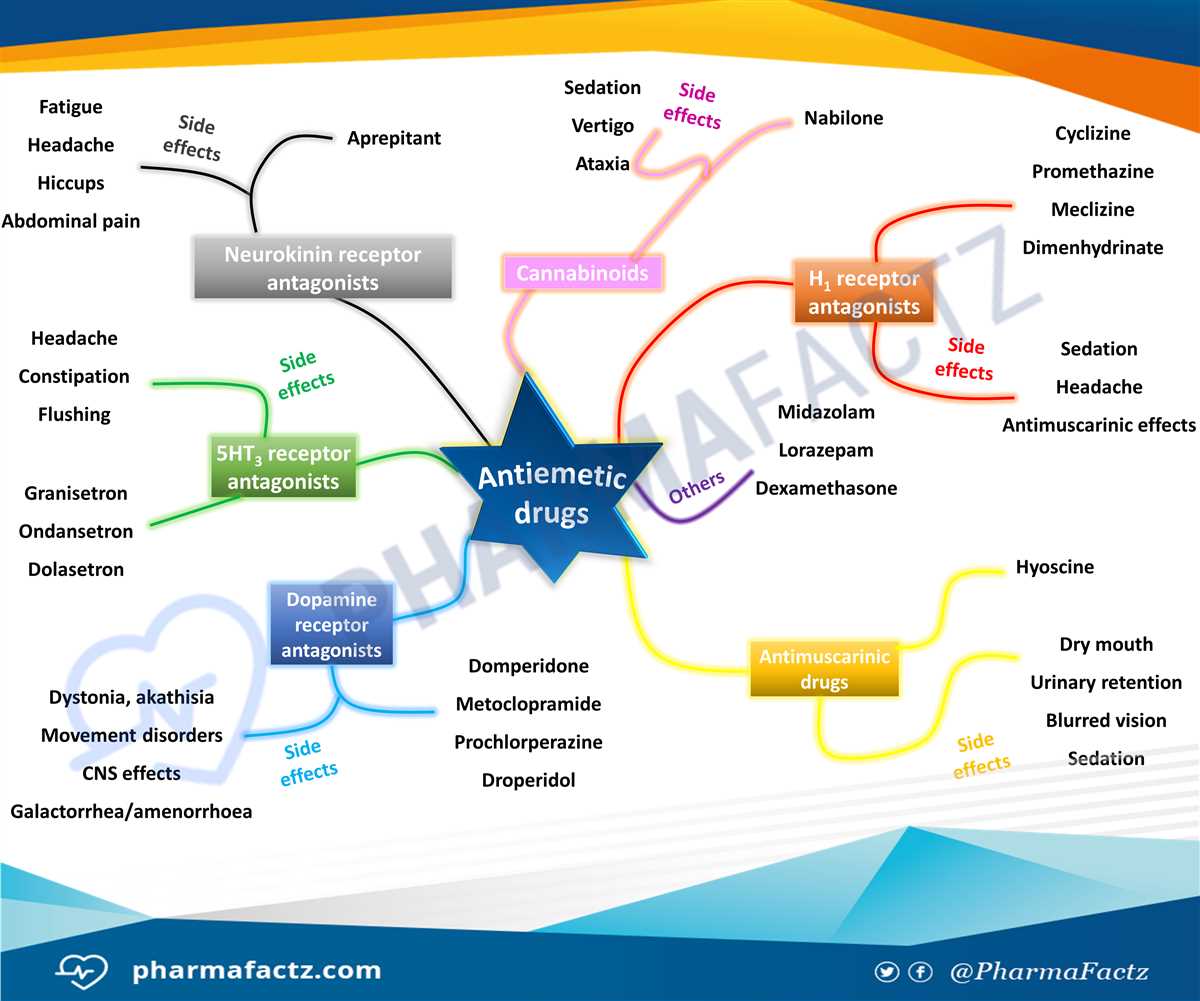
As the end of the semester approaches, it’s time to prepare for the final exam in pharmacology. This study guide aims to help students review key concepts, drug classifications, and therapeutic uses to ensure success on the upcoming test. Pharmacology is a crucial subject for healthcare professionals as it involves the study of how drugs interact with the body to treat, manage, and prevent diseases.
In this study guide, students will find a comprehensive overview of the major drug classes, including the mechanisms of action, side effects, and contraindications for each. The guide will also delve into the principles of pharmacokinetics and pharmacodynamics, explaining how drugs are absorbed, distributed, metabolized, and excreted by the body, as well as how they exert their therapeutic effects.
Furthermore, this study guide will cover important topics such as drug interactions, adverse drug reactions, and the principles of rational drug selection. It will provide students with essential knowledge on how to evaluate the safety and efficacy of different drugs and make informed decisions when prescribing or administering medications.
By thoroughly reviewing this study guide and actively engaging in self-assessment exercises, students will be well-prepared to excel on the pharmacology final exam and lay a solid foundation for their future careers in healthcare.
Pharmacology Final Exam Study Guide: Everything You Need to Know

In preparation for your pharmacology final exam, it is essential to have a comprehensive study guide that covers all the important topics and concepts. This guide will provide you with a detailed overview of the key points you need to know to succeed in your exam.
1. Drug Classification: Familiarize yourself with the different drug classes and their mechanisms of action. Understand the specific drugs within each class and their therapeutic uses.
2. Pharmacokinetics: Study the processes involved in drug absorption, distribution, metabolism, and elimination. Learn the factors that affect drug pharmacokinetics and how to interpret pharmacokinetic parameters.
3. Pharmacodynamics: Understand how drugs interact with receptors and other targets in the body. Learn the different types of drug-receptor interactions, including agonists, antagonists, and inverse agonists.
- 4. Drug Interactions: Learn about potential drug-drug interactions and how they can impact drug therapy. Understand the mechanisms of drug interactions and how to manage them to ensure patient safety.
- 5. Adverse Drug Reactions: Study the common side effects and adverse reactions associated with different drug classes. Learn how to identify and manage these reactions to provide optimal patient care.
- 6. Dosage Calculations: Practice calculating drug dosages based on patient factors such as weight, age, and renal function. Understand the different dosage forms and routes of administration.
7. Therapeutic Drug Monitoring: Familiarize yourself with the concept of therapeutic drug monitoring and its importance in optimizing drug therapy. Learn how to interpret drug levels and adjust dosages accordingly.
| 8. Drug Safety: | 9. Pharmacogenetics: |
|---|---|
| Understand the principles of medication safety, including medication errors, adverse drug events, and strategies to prevent medication-related harm. | Study the role of genetics in drug response and how genetic variations can influence individual responses to medications. Be aware of pharmacogenomic testing and its implications in personalized medicine. |
10. Drug Regulation and Ethics: Learn about the laws and regulations governing the development, approval, and marketing of drugs. Understand the ethical considerations in pharmacology, including informed consent and patient autonomy.
With this comprehensive study guide, you will be well-equipped to tackle your pharmacology final exam. Remember to review your class notes, textbooks, and practice with sample questions to reinforce your understanding of the subject matter. Good luck!
Understanding Drug Classification and their Mechanisms of Action
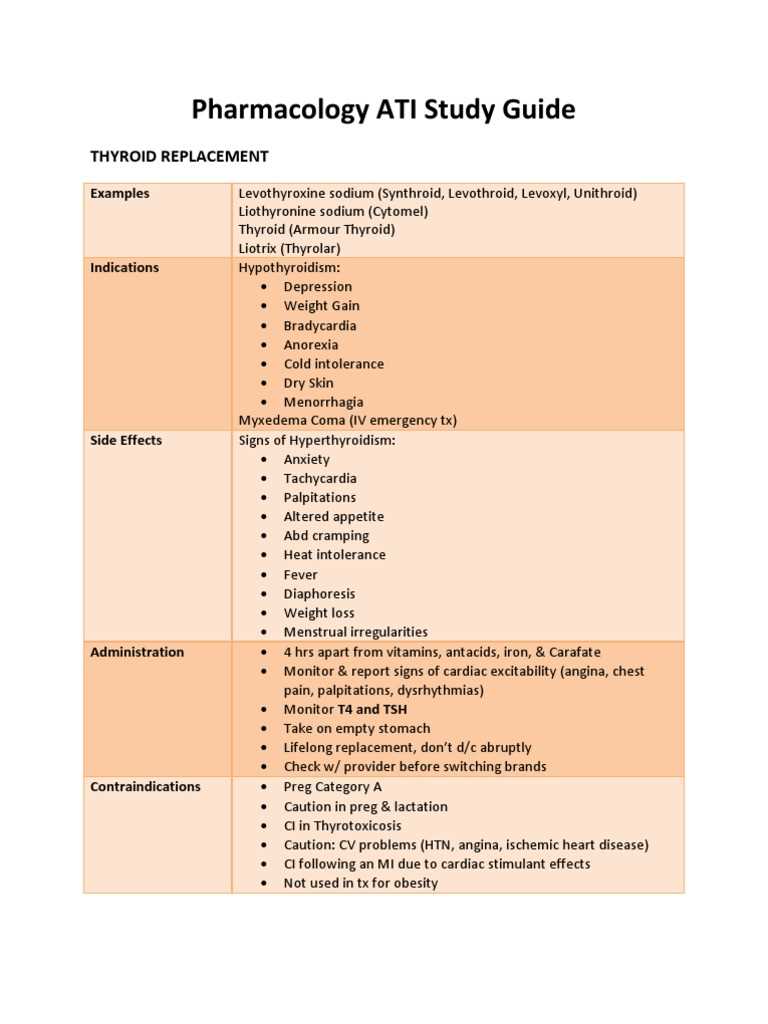
Drug classification is an important aspect of pharmacology, as it allows healthcare professionals and researchers to categorize drugs based on their therapeutic uses and mechanisms of action. By understanding the classification of drugs, healthcare professionals can make informed decisions about drug therapy and predict potential drug interactions and side effects.
There are several ways to classify drugs, including their chemical structure, therapeutic use, and mechanism of action. One common classification system is based on a drug’s mechanism of action, which refers to how the drug interacts with specific molecular targets in the body to produce its therapeutic effects.
Drug classification based on mechanism of action:
- Agonists: Drugs that bind to and activate specific receptors in the body, mimicking the effects of endogenous substances.
- Antagonists: Drugs that bind to receptors without activating them, blocking the effects of endogenous substances.
- Enzyme inhibitors: Drugs that inhibit the activity of specific enzymes, preventing or reducing the production of certain substances in the body.
- Ion channel blockers: Drugs that block specific ion channels in cell membranes, affecting the flow of ions and altering cell function.
- Transporter inhibitors: Drugs that inhibit the activity of specific transporters in cell membranes, affecting the transport of substances across the cell membrane.
Understanding drug classification based on mechanism of action is crucial for healthcare professionals to make appropriate prescribing decisions and monitor patients for potential drug interactions and side effects. It also provides a foundation for future drug development and research.
Commonly Used Pharmacological Agents: their Uses and Side Effects
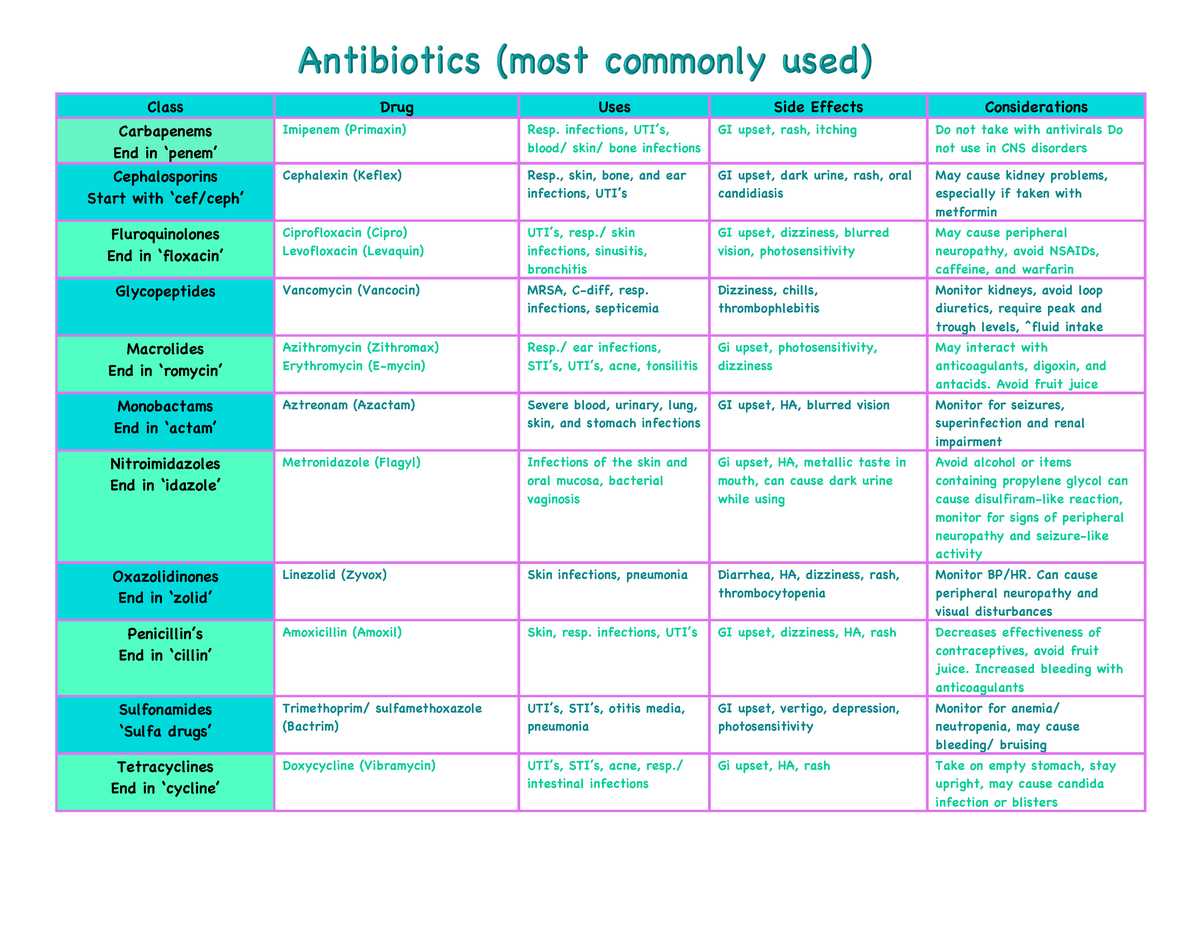
Pharmacological agents, also known as drugs or medications, are commonly used in medical practice to treat various conditions and diseases. These agents can have different uses and can be classified into different categories based on their mechanism of action. It is important for healthcare professionals to have a good understanding of these agents and their potential side effects in order to ensure safe and effective use.
Antibiotics: Antibiotics are drugs used to treat bacterial infections. They work by either killing the bacteria or inhibiting their growth. Some commonly used antibiotics include penicillin, amoxicillin, and ciprofloxacin. While antibiotics are effective in treating bacterial infections, they can also have side effects such as allergic reactions, diarrhea, and nausea.
Analgesics: Analgesics, also known as painkillers, are drugs used to relieve pain. They can be classified into different categories, such as nonsteroidal anti-inflammatory drugs (NSAIDs) and opioids. NSAIDs, such as ibuprofen and aspirin, work by reducing inflammation and relieving pain. Opioids, such as morphine and oxycodone, act on the central nervous system to reduce the perception of pain. However, these drugs can also cause side effects such as drowsiness, constipation, and addiction.
- Antidepressants: Antidepressants are drugs used to treat depression and other mood disorders. They work by increasing the levels of certain neurotransmitters in the brain. Selective serotonin reuptake inhibitors (SSRIs), such as fluoxetine and sertraline, are commonly prescribed antidepressants. Side effects of antidepressants can include nausea, sexual dysfunction, and weight gain.
- Antihypertensives: Antihypertensives are drugs used to treat high blood pressure. They work by relaxing the blood vessels and reducing the workload on the heart. Some commonly used antihypertensives include angiotensin-converting enzyme (ACE) inhibitors, beta blockers, and diuretics. Side effects of antihypertensives can include dizziness, fatigue, and dry cough.
- Antidiabetic agents: Antidiabetic agents are drugs used to manage diabetes by controlling blood sugar levels. They can be classified into different categories, such as insulin and oral hypoglycemic agents. Insulin is a hormone that regulates blood sugar levels, while oral hypoglycemic agents help the body use insulin more effectively. Side effects of antidiabetic agents can include hypoglycemia, weight gain, and gastrointestinal disturbances.
These are just a few examples of commonly used pharmacological agents and their uses and side effects. It is important to consult with a healthcare professional for specific information about a particular drug and its potential side effects.
Pharmacokinetics and Pharmacodynamics: How Drugs are Absorbed, Distributed, Metabolized, and Eliminated in the Body
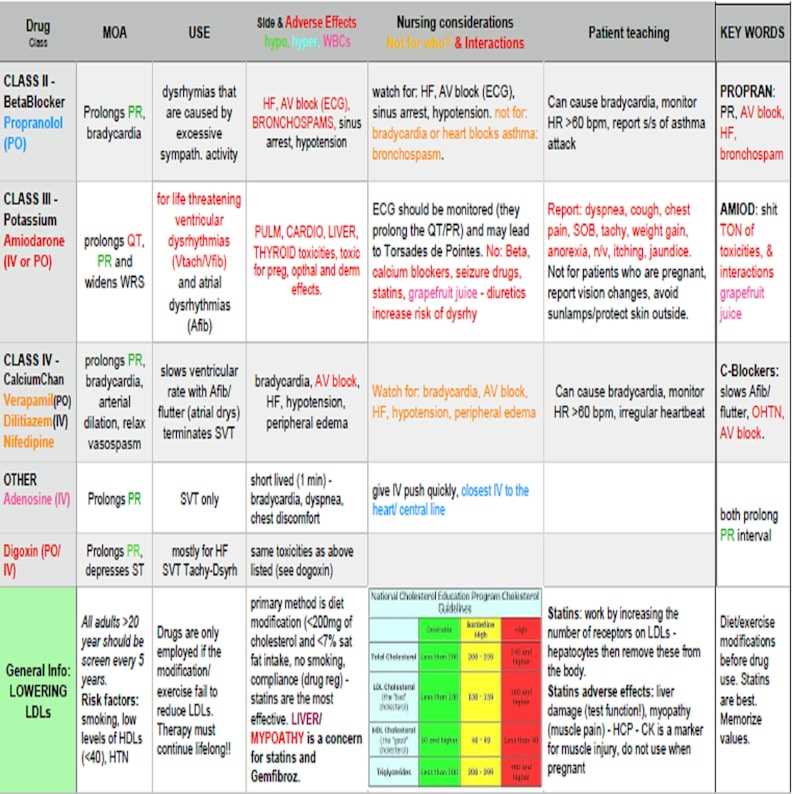
Pharmacokinetics and pharmacodynamics are two essential concepts in the field of pharmacology that help explain how drugs interact with the body. Pharmacokinetics refers to the study of how a drug is absorbed, distributed, metabolized, and eliminated in the body, while pharmacodynamics focuses on the effects of the drug on the body and the relationship between drug concentration and its pharmacological effects.
In terms of absorption, drugs can enter the body through different routes, including oral ingestion, inhalation, injection, and topical application. Once in the body, the drug’s absorption process may vary depending on factors such as the drug’s physicochemical properties, the route of administration, and the presence of food or other drugs. For example, oral drugs need to pass through the gastrointestinal tract, where they may be affected by gastric acidity and enzymatic degradation before reaching systemic circulation.
After absorption, the drug is distributed throughout the body via the bloodstream. Various factors, such as drug size, lipophilicity, protein binding, and tissue perfusion, can influence its distribution. Drugs may bind to plasma proteins, such as albumin, which can affect their distribution and duration of action. Additionally, drugs can cross different barriers, such as the blood-brain barrier or the placental barrier, leading to specific pharmacological effects or potential risks in certain populations.
Metabolism plays a crucial role in drug clearance and elimination. The liver is the primary site of drug metabolism, where enzymes break down the drug into metabolites that can be more easily excreted. This process, known as biotransformation, can lead to both activation and inactivation of drugs. The hepatic enzymes responsible for drug metabolism include cytochrome P450 enzymes, which are involved in the metabolism of a wide range of drugs. However, some drugs can also undergo metabolism in other organs or tissues.
Finally, drugs are eliminated from the body through various routes, such as renal excretion (via urine), biliary excretion (via feces), or through the lungs (via exhaled air). The rate of drug elimination can be influenced by factors such as renal function, age, and drug interactions. Understanding the pharmacokinetic and pharmacodynamic properties of drugs is essential in determining the appropriate dosage, frequency, and duration of drug therapy, as well as predicting potential drug-drug or drug-disease interactions.
Drug Interactions: Understanding Potential Adverse Effects and Avoiding Harmful Combinations
Drug interactions occur when two or more medications, or a medication and another substance, interact with each other and produce a modified effect. These interactions can result in either beneficial or harmful outcomes. It is important for healthcare professionals and patients to be aware of potential drug interactions to avoid adverse effects and ensure optimal therapeutic outcomes.
Potential adverse effects: Drug interactions can lead to various adverse effects, ranging from mild to life-threatening. These effects may include increased or decreased drug concentrations in the body, altered metabolism or elimination, changes in drug efficacy, and enhanced or reduced drug toxicity. Some common adverse effects of drug interactions include increased risk of side effects, reduced therapeutic efficacy, drug resistance, organ toxicity, and drug-induced allergic reactions.
Avoiding harmful combinations: To avoid harmful drug combinations, healthcare professionals should consider the following strategies:
- Thoroughly review the patient’s medical history and medication list to identify potential drug interactions.
- Consult reliable drug interaction databases or reference sources to assess the likelihood and severity of possible interactions.
- Consider the pharmacokinetic and pharmacodynamic properties of the drugs involved, including their absorption, distribution, metabolism, and excretion.
- Adjust the dosage or timing of administration if necessary, based on the potential interaction.
- Closely monitor the patient for any signs or symptoms of drug interactions or adverse effects.
By applying these strategies, healthcare professionals can minimize the risk of harmful drug interactions and ensure safe and effective medication use for their patients.
Principles of Medication Administration and Dosage Calculations

Medication administration is a critical skill in pharmacology, as it involves the safe and accurate delivery of medications to patients. It is essential for healthcare professionals to follow certain principles in order to ensure patient safety and optimize therapeutic outcomes.
1. The Five Rights: One of the fundamental principles of medication administration is the concept of the “Five Rights”. This includes administering the right medication, to the right patient, in the right dose, via the right route, at the right time. Following these principles reduces the risk of medication errors and ensures that patients receive the appropriate treatment.
2. Dosage Calculations: Healthcare professionals are responsible for accurately calculating medication dosages based on a patient’s specific needs. This involves understanding the prescribed medication’s concentration, the patient’s weight, and any other relevant factors. Different calculation methods, such as ratio and proportion or dimensional analysis, may be used to determine the correct dosage for administration.
3. Administration Techniques: There are various routes of medication administration, including oral, subcutaneous, intramuscular, intravenous, and topical. Each route requires specific techniques to ensure proper absorption and minimize adverse effects. Healthcare professionals must be knowledgeable about these techniques and follow appropriate guidelines for each route of administration.
4. Safety Precautions: Medication administration involves taking precautions to prevent harm to patients. This includes checking medication labels for accuracy, verifying patient allergies and contraindications, and performing safety checks throughout the administration process. Proper documentation and communication between healthcare professionals are also essential to prevent medication errors and ensure patient safety.
5. Patient Education: In addition to administering medications, healthcare professionals play a vital role in educating patients about their medications. This includes explaining the purpose of the medication, potential side effects, and proper administration techniques. Patient education is crucial for promoting medication adherence and empowering patients to participate in their own healthcare.