
When assessing the health of a patient’s ears, it is crucial for healthcare providers to document their findings accurately. Proper documentation of a normal ear exam allows for a baseline reference in case any changes occur in the future. This article aims to discuss the essential components of documenting a normal ear exam in a medical setting.
First and foremost, a comprehensive description of the external ear is necessary. This includes noting the size, shape, and symmetry of the pinna and the presence of any abnormalities or lesions. Additionally, the condition of the ear canal should be documented, such as its color, presence of cerumen, and any signs of inflammation.
Next, it is vital to document the findings of the otoscopic examination. This involves visualizing the tympanic membrane and the middle ear structures. Healthcare providers should describe the appearance and position of the tympanic membrane, looking for signs of infection, perforation, or effusion. Furthermore, the mobility of the tympanic membrane should be assessed using pneumatic otoscopy.
Finally, it is necessary to document the results of any additional tests performed during the ear exam. This may include audiometry, where the patient’s hearing thresholds are assessed, or tympanometry, which evaluates the middle ear function. The results of these tests should be transcribed accurately, including any abnormalities or deviations from normal.
In conclusion, documenting a normal ear exam is an essential aspect of patient care, ensuring that any changes in ear health can be identified and addressed promptly. Through comprehensive descriptions of the external ear, otoscopic examination findings, and additional test results, healthcare providers can maintain a comprehensive record of the patient’s ear health over time.
Why is Ear Exam Documentation Important?
Ear exam documentation is crucial for several reasons. Firstly, it provides a detailed record of the patient’s ear health and any abnormalities that may be present. This documentation serves as a reference for future visits and allows healthcare professionals to track changes in the patient’s condition over time.
Furthermore, ear exam documentation is essential for communication between healthcare providers. By documenting the findings of the ear exam, healthcare professionals can easily share information with other specialists, ensuring continuity of care and facilitating collaboration in determining the best treatment plan.
Accurate and thorough ear exam documentation is also important for medico-legal purposes. In the event of a lawsuit or dispute, the documented findings can serve as evidence to support the healthcare provider’s actions and decisions. It can also protect against claims of negligence or improper treatment.
In addition, ear exam documentation contributes to research and medical education. By documenting patient cases and outcomes, medical professionals can contribute to the advancement of knowledge and the development of more effective diagnostic and treatment methods for ear conditions.
What to Include in Ear Exam Documentation
The documentation of an ear exam is a crucial part of a patient’s medical record. It provides a detailed account of the examination findings, helping healthcare professionals in diagnosis and treatment planning. When documenting an ear exam, the following information should be included:
I. Patient Information
- Full name and age of the patient
- Any relevant medical history, such as previous ear infections or surgeries
II. Examination Technique
- The type of examination conducted, such as otoscopy, audiometry, or tympanometry
- The instruments or equipment used during the examination
III. Examination Findings
- A detailed description of the external ear, including the presence of any abnormalities, lesions, or swelling
- An evaluation of the ear canal, noting any signs of infection, inflammation, or cerumen impaction
- An assessment of the tympanic membrane, including its color, position, and any signs of effusion or perforation
- If applicable, results of audiometric tests, such as the patient’s threshold and speech discrimination scores
IV. Interpretation and Impression
- An interpretation of the examination findings, relating them to the patient’s symptoms and medical history
- A provisional or final diagnosis, if possible, based on the examination findings
- Any recommendations for further investigation or treatment
V. Conclusion
Make sure to conclude the documentation by signing and dating it, indicating the name or initials of the healthcare professional who performed the examination.
Step-by-step Guide to Conducting an Ear Exam

An ear exam is an important diagnostic procedure that allows healthcare providers to assess the health of the ears, identify any abnormalities, and determine the appropriate course of treatment. Here is a step-by-step guide to conducting an ear exam:
Step 1: Patient preparation
- Instruct the patient to remove any earrings or other objects from the ears.
- Explain the procedure to the patient and address any concerns or questions they may have.
Step 2: Visual examination of the external ear
- Inspect the external ear for any abnormalities such as redness, swelling, discharge, or lesions.
- Pull the ear gently backward and upward to straighten the ear canal for better visibility.
- Use a penlight or otoscope to examine the external ear canal and the eardrum.
Step 3: Evaluation of the ear canal and eardrum

- Assess the condition of the ear canal, noting any cerumen (ear wax) buildup, foreign bodies, or signs of infection.
- Examine the eardrum for its color, integrity, position, and any signs of perforation or fluid accumulation.
- Record any findings, such as the presence of redness, bulging, retraction, or tympanic membrane mobility.
Step 4: Assessment of auditory function
- Conduct a hearing test to evaluate the patient’s ability to perceive different sound frequencies and intensities.
- Use an audiometer or other appropriate equipment to measure the patient’s hearing thresholds.
- Document the test results and compare them to normal values.
Step 5: Additional tests or referrals
- If necessary, perform additional tests such as tympanometry or acoustic reflex testing to gather more information about the middle ear function.
- Refer the patient to an audiologist or otolaryngologist for further evaluation if significant abnormalities are detected.
By following these steps, healthcare providers can conduct a thorough ear exam and gather the necessary information for accurate diagnosis and appropriate treatment planning.
Tools and Equipment Needed for Ear Exam Documentation
When conducting an ear exam, it is crucial to have the proper tools and equipment to accurately document the findings. These tools not only aid in the examination process but also allow for detailed documentation that can be utilized for future reference. Some essential tools for ear exam documentation include:
- Otoscope: An otoscope is a hand-held instrument with a light and magnifying lens that allows healthcare professionals to examine the external ear canal and eardrum. It is vital for assessing the overall condition of the ear and documenting any abnormalities.
- Tympanometer: A tympanometer is a diagnostic tool that measures the movement of the eardrum in response to changes in air pressure. It provides objective data about middle ear function and can be used to document any abnormalities or issues.
- Speculum: A speculum is a device that is inserted into the ear canal to help visualize the eardrum and surrounding structures. It comes in various sizes and shapes to accommodate different ear sizes and allows for a clearer view during the examination.
- Cotton swabs: Cotton swabs are used for cleaning the external ear and removing any excess wax or debris. They should be used with caution and only for cleaning the outer ear, as inserting them into the ear canal can cause damage or push wax further into the ear.
- Medical grade gloves: Wearing medical grade gloves is essential to maintain hygiene during the ear exam. It helps prevent the spread of infections and ensures patient safety.
Having these tools and equipment readily available during an ear exam allows healthcare professionals to accurately document the condition of the ear and provide appropriate treatment or referrals if necessary. Proper documentation is essential for keeping accurate medical records and ensuring continuity of care for the patient.
Common Findings and Abnormalities in Ear Exam Documentation
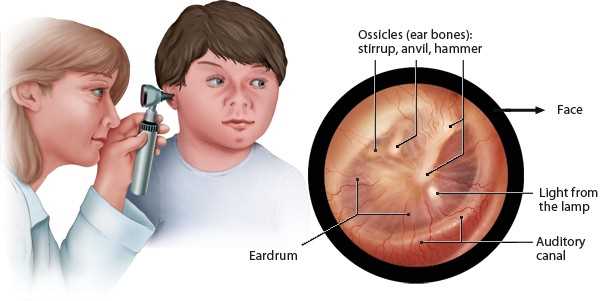
The examination of the ear is a crucial aspect of a routine physical examination. During an ear exam, healthcare professionals often encounter various common findings and abnormalities that require documentation for accurate diagnosis and treatment planning.
Common Findings:
- Normal tympanic membrane: A normal tympanic membrane appears pearly gray in color with a intact light reflex, and it is considered a common finding during an ear examination.
- Clear ear canal: A clear ear canal without any signs of obstruction or excessive earwax buildup is also a commonly found during an ear exam.
- Normal auditory acuity and response: A common finding is a normal hearing ability and appropriate response to sound stimuli during a hearing test.
- Absence of abnormal discharge: Lack of abnormal discharge, such as blood or pus, from the ear is another common finding that indicates a healthy condition.
Abnormalities:
- Otitis media: Otitis media is a common abnormality characterized by inflammation and infection of the middle ear. It often presents with symptoms such as ear pain, fever, and fluid accumulation behind the eardrum.
- Tympanic membrane perforation: Tympanic membrane perforation is an abnormality that involves a tear or hole in the eardrum. It can be caused by trauma, infection, or changes in pressure and may result in hearing loss and recurrent ear infections.
- Foreign body presence: Another abnormality during an ear exam is the presence of a foreign body, such as an insect or small object, lodged in the ear canal. This requires immediate removal to prevent complications.
- Impacted earwax: Excessive earwax buildup leading to obstruction of the ear canal is a common abnormality encountered during an ear exam. It can cause hearing loss and discomfort.
In conclusion, documenting the common findings and abnormalities observed during an ear exam is essential in order to provide accurate diagnoses and appropriate treatment plans for patients. It allows healthcare professionals to monitor any changes in the ear’s condition and ensure optimal ear health.
How to Document Normal Findings in an Ear Exam
When conducting an ear exam, it is important to document any findings, whether they are normal or abnormal. Documenting normal findings helps establish a baseline for future reference and ensures accurate patient records. Here are some tips on how to document normal findings in an ear exam:
- Inspect the external ear: Begin by visually examining the external ear for any abnormalities. Note the presence of any skin lesions, swelling, or deformities. Document the findings accordingly.
- Assess the ear canal: Use an otoscope to examine the ear canal. Note the presence of cerumen or debris, as well as the overall condition of the ear canal wall. Document any normal findings or abnormalities observed.
- Examine the tympanic membrane: Carefully inspect the tympanic membrane using the otoscope. Note its color, position, and integrity. Document any normal findings, such as a pearly gray color and an intact membrane.
- Test hearing: Conduct a basic hearing test to assess the patient’s ability to hear different frequencies and volumes. Use a tuning fork or audiometer to determine if the patient’s hearing falls within the normal range. Document the results of the hearing test.
- Evaluate middle ear function: Perform a pneumatic otoscopy to assess the movement of the tympanic membrane. Observe the normal movement of the membrane in response to changes in pressure. Document any normal findings or abnormalities.
By thoroughly documenting normal findings in an ear exam, healthcare professionals can accurately track changes in a patient’s ear health over time. This documentation also serves as a reference for future healthcare providers who may need to review the patient’s medical history. Proper documentation ensures comprehensive and high-quality patient care.
Importance of Accurate and Detailed Ear Exam Documentation

The accurate and detailed documentation of an ear exam is crucial for several reasons. Firstly, it provides a comprehensive record of the patient’s ear health, allowing healthcare professionals to monitor any changes or developments over time. This documentation can be especially important for patients with chronic conditions or those who require long-term follow-up.
Accurate documentation also plays a vital role in communication between healthcare providers. When different clinicians are involved in a patient’s care, having access to detailed ear exam documentation can help ensure continuity and consistency in treatment. It enables healthcare professionals to understand the patient’s condition, track progress, and make informed decisions regarding further diagnostic tests or treatment options.
Moreover, meticulous ear exam documentation is crucial from a medicolegal standpoint. In the event of a medical malpractice claim or dispute, detailed records can provide evidence of the care provided and help in determining the appropriateness of treatment. It can also serve as invaluable information for research studies and quality improvement initiatives, aiding in the development and evaluation of best practices in ear care.
To ensure accurate and detailed ear exam documentation, healthcare professionals should include relevant information such as the patient’s medical history, symptoms, examination findings, diagnostic tests performed, treatment provided, and follow-up plans. They should also use standardized terminology and codes to facilitate clear and consistent communication. Adopting electronic health record systems can further enhance the accuracy and accessibility of ear exam documentation.
- Key Points:
- Accurate and detailed ear exam documentation allows for monitoring changes in ear health over time.
- It facilitates communication between healthcare providers and ensures continuity of care.
- Documentation is crucial for medicolegal purposes and research initiatives.
- Including relevant information and using standardized terminology improves the quality of documentation.
- Electronic health record systems enhance accuracy and accessibility.