
The American Heart Association (AHA) is set to release the updated guidelines for Advanced Cardiovascular Life Support (ACLS) in 2024. These guidelines serve as the foundation for the written exam that healthcare professionals must pass in order to become ACLS certified.
The ACLS written exam is a comprehensive assessment that evaluates the knowledge and skills of healthcare providers in managing cardiac emergencies. It covers a wide range of topics, including recognition and treatment of cardiac arrest, rhythm recognition, pharmacology, and team dynamics.
The 2024 exam is expected to incorporate the latest research and evidence-based practices in the field of ACLS. Healthcare providers will need to stay up-to-date with the new guidelines and ensure that they are familiar with any changes that may be introduced. This will require ongoing education and training to ensure that providers are equipped to provide the best possible care to patients in cardiac emergencies.
Passing the ACLS written exam is an important milestone for healthcare professionals as it demonstrates their proficiency in managing critical situations. It is a testament to their dedication to patient care and commitment to continuous learning and improvement.
As the field of ACLS continues to evolve, it is vital for healthcare providers to stay informed and prepared for any new challenges that may arise. The 2024 ACLS written exam will serve as a benchmark for healthcare providers, ensuring that they possess the necessary knowledge and skills to save lives during cardiac emergencies.
Acls Written Exam 2024
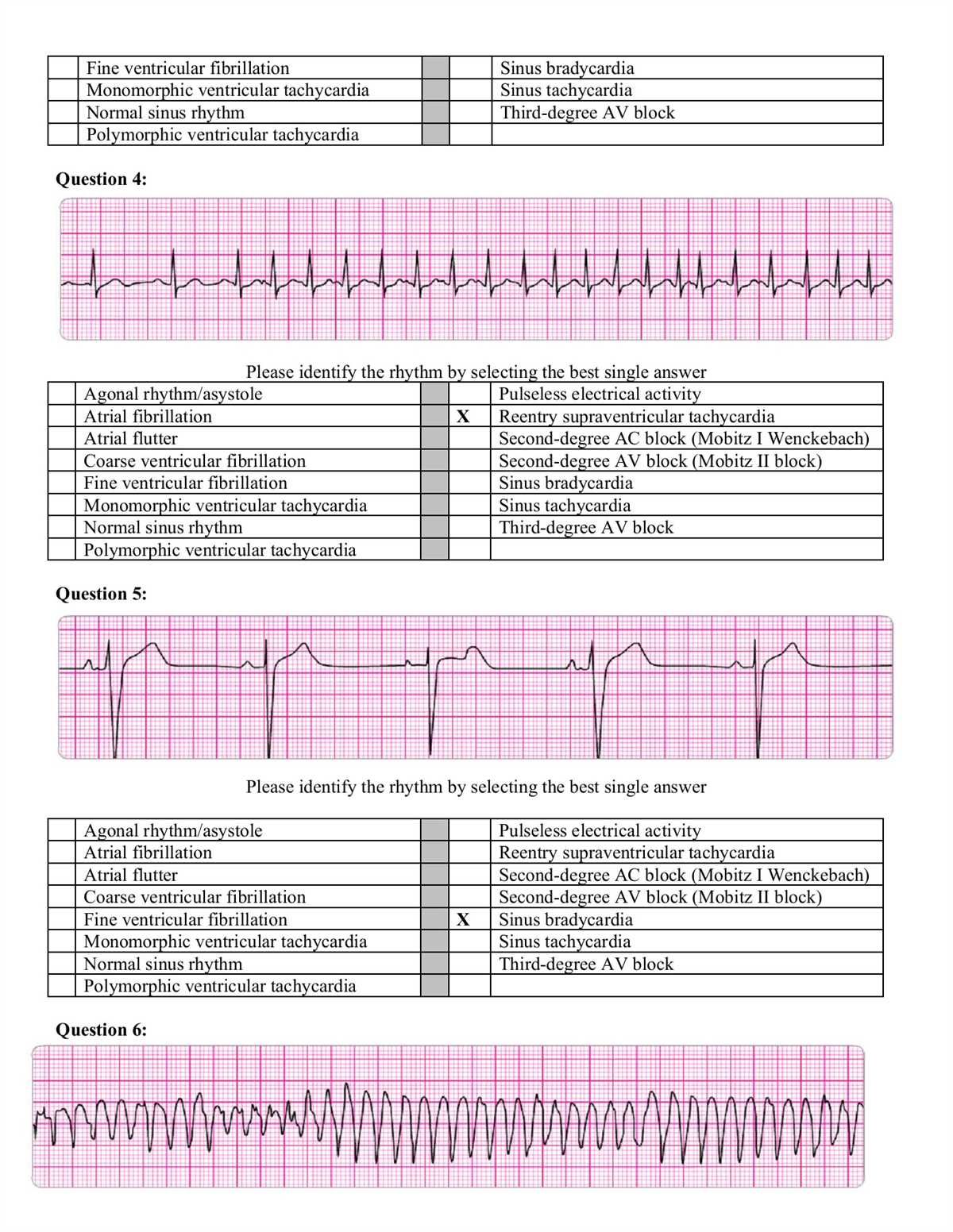
The ACLS Written Exam for the year 2024 is an important assessment that evaluates the knowledge and skills of healthcare professionals in managing advanced cardiac life support situations. This exam is designed to ensure that healthcare providers have the necessary abilities to respond effectively to cardiac emergencies and provide the best possible care to patients.
During the ACLS Written Exam 2024, participants will be tested on various topics, including recognizing and interpreting cardiac rhythms, understanding the use of medications and electrical therapies, and implementing ACLS algorithms in different scenarios. This exam requires a thorough understanding of ACLS guidelines and protocols, as well as the ability to make quick decisions and communicate effectively in high-stress situations.
Test-takers will encounter a combination of multiple-choice questions and scenario-based questions that simulate real-life emergency situations. They will need to demonstrate their knowledge of ACLS principles, identify appropriate interventions, and prioritize patient care based on the severity of the condition. The ACLS Written Exam 2024 aims to assess the critical thinking skills and clinical judgment of healthcare providers and ensure they are well-prepared to handle cardiac emergencies.
Key Topics Covered in the ACLS Written Exam 2024:
- Cardiac rhythms and their interpretation
- Pharmacology and medication administration during ACLS
- Electrical therapies, including defibrillation and cardioversion
- ACLS algorithms for different emergency scenarios
- Team dynamics and effective communication in high-stress situations
- Post-resuscitation care and monitoring
Successful completion of the ACLS Written Exam 2024 is a significant achievement for healthcare professionals, as it demonstrates their competency and readiness to provide advanced cardiac life support. It is essential to study and review the relevant guidelines, algorithms, and procedures before taking the exam to ensure a confident and successful performance.
Understanding the ACLS Certification Process
If you are looking to become certified in Advanced Cardiovascular Life Support (ACLS), it is important to understand the certification process. ACLS certification is a specialized training program designed for healthcare professionals who may be involved in the resuscitation and management of cardiac arrest and other cardiovascular emergencies.
ACLS certification involves both theoretical knowledge and practical skills training. The certification process typically consists of completing a comprehensive ACLS course, which covers topics such as the recognition and treatment of cardiac arrest, rhythm disturbances, respiratory emergencies, and post-cardiac arrest care. The course may also include demonstrations and hands-on practice sessions to develop skills in performing advanced cardiovascular life support interventions.
After completing the ACLS course, you will need to pass a written exam to demonstrate your understanding of the ACLS algorithms, pharmacology, and clinical scenarios. The exam usually consists of multiple-choice questions and requires a passing score to receive certification. Additionally, some certification programs may require you to complete a skills evaluation, where you will be assessed on your ability to perform ACLS interventions correctly and efficiently.
Once you successfully complete the ACLS certification process, you will be issued a certificate that is valid for a certain period, typically two years. To maintain your certification, you will need to renew it before it expires by completing a recertification course or exam. Recertification ensures that healthcare professionals stay up to date with the latest guidelines and best practices in ACLS to provide the highest level of care to patients in cardiovascular emergencies.
In conclusion, the ACLS certification process involves completing a comprehensive course, passing a written exam, and potentially undergoing a skills evaluation. Certification is valid for a specified period, and recertification is necessary to ensure ongoing competence and proficiency in ACLS. By obtaining and maintaining ACLS certification, healthcare professionals can play a crucial role in saving lives during cardiac emergencies.
Important Updates for the ACLS Written Exam in 2024
The ACLS (Advanced Cardiovascular Life Support) written exam in 2024 will feature several important updates aimed at ensuring that healthcare professionals possess the necessary skills and knowledge to provide effective life-saving interventions in emergency situations. These updates reflect the latest guidelines and evidence-based practices in resuscitation and cardiac care.
1. Expanded focus on high-quality CPR: CPR is a critical component of ACLS, and the exam in 2024 will emphasize the importance of providing high-quality CPR. Candidates will be tested on their ability to perform effective chest compressions, maintain proper ventilation, and use an AED (automated external defibrillator) correctly.
2. Enhanced emphasis on team dynamics: Effective teamwork is vital in the management of cardiac arrest and other emergency situations. The ACLS written exam will evaluate candidates’ understanding of team roles and responsibilities, communication strategies, and the ability to lead and follow within a resuscitation team.
- 3. Updated algorithms and protocols: The exam will incorporate the most recent updates to the ACLS algorithms and protocols. Candidates should be familiar with the latest guidelines for the management of specific cardiac rhythms, drug administration, and post-cardiac arrest care.
- 4. Integration of technology: The use of technology in resuscitation is evolving rapidly. Candidates will be tested on their ability to utilize advanced devices and technologies, such as mechanical CPR devices and capnography, in accordance with current best practices.
- 5. Comprehensive knowledge assessment: The ACLS written exam will assess candidates’ understanding of the underlying pathophysiology of cardiovascular emergencies, pharmacology, and electrocardiogram (ECG) interpretation. It will also include questions related to special populations, such as pediatric and geriatric patients.
These updates aim to ensure that healthcare professionals are well-prepared to provide optimal care to patients in critical situations. It is crucial for candidates to stay updated with the latest guidelines and evidence-based practices in ACLS to succeed in the exam and deliver the highest quality of care.
Key Concepts and Guidelines in ACLS
Advanced Cardiac Life Support (ACLS) is a set of guidelines and protocols designed to provide medical practitioners with a systematic approach to addressing cardiac emergencies. These key concepts and guidelines are crucial for healthcare professionals to effectively manage and treat patients with life-threatening cardiac conditions.
1. Basic Life Support (BLS) and Early Defibrillation: Prompt initiation of Basic Life Support, including chest compressions and early defibrillation, is essential in the management of cardiac arrest. BLS serves as the foundation for ACLS protocols and should be initiated within minutes of identifying cardiac arrest.
2. Primary and Secondary Assessment: ACLS follows a systematic approach to patient assessment, involving primary and secondary assessments. The primary assessment focuses on recognizing and addressing immediate life-threatening conditions, such as airway obstruction or inadequate breathing, while the secondary assessment involves a more comprehensive evaluation of the patient’s condition and identifying the underlying cause of the cardiac event.
- 3. Algorithms: ACLS utilizes algorithms to guide healthcare professionals through the management of specific cardiac rhythms and conditions. These algorithms provide step-by-step instructions on interventions such as defibrillation, drug administration, and advanced airway management.
- 4. Medications: ACLS provides guidelines for the administration of medications during cardiac emergencies. These medications include antiarrhythmics, vasopressors, and adjunctive therapies designed to stabilize cardiac rhythms and improve perfusion.
- 5. Advanced Airway Management: ACLS guidelines outline approaches to advanced airway management, including endotracheal intubation and supraglottic airway devices, for patients who require ventilatory support during resuscitation.
6. Team Dynamics and Communication: Effective communication and coordination within the resuscitation team are critical in ACLS scenarios. Clear roles and responsibilities, closed-loop communication, and regular updates ensure seamless patient care and optimal resuscitation outcomes.
7. Post-Cardiac Arrest Care: ACLS emphasizes the importance of post-cardiac arrest care, including targeted temperature management, hemodynamic optimization, and immediate identification and treatment of the underlying cause of the cardiac event. These interventions aim to improve the patient’s overall prognosis and reduce the risk of recurrent cardiac events.
Reviewing Cardiac Arrest Management in ACLS
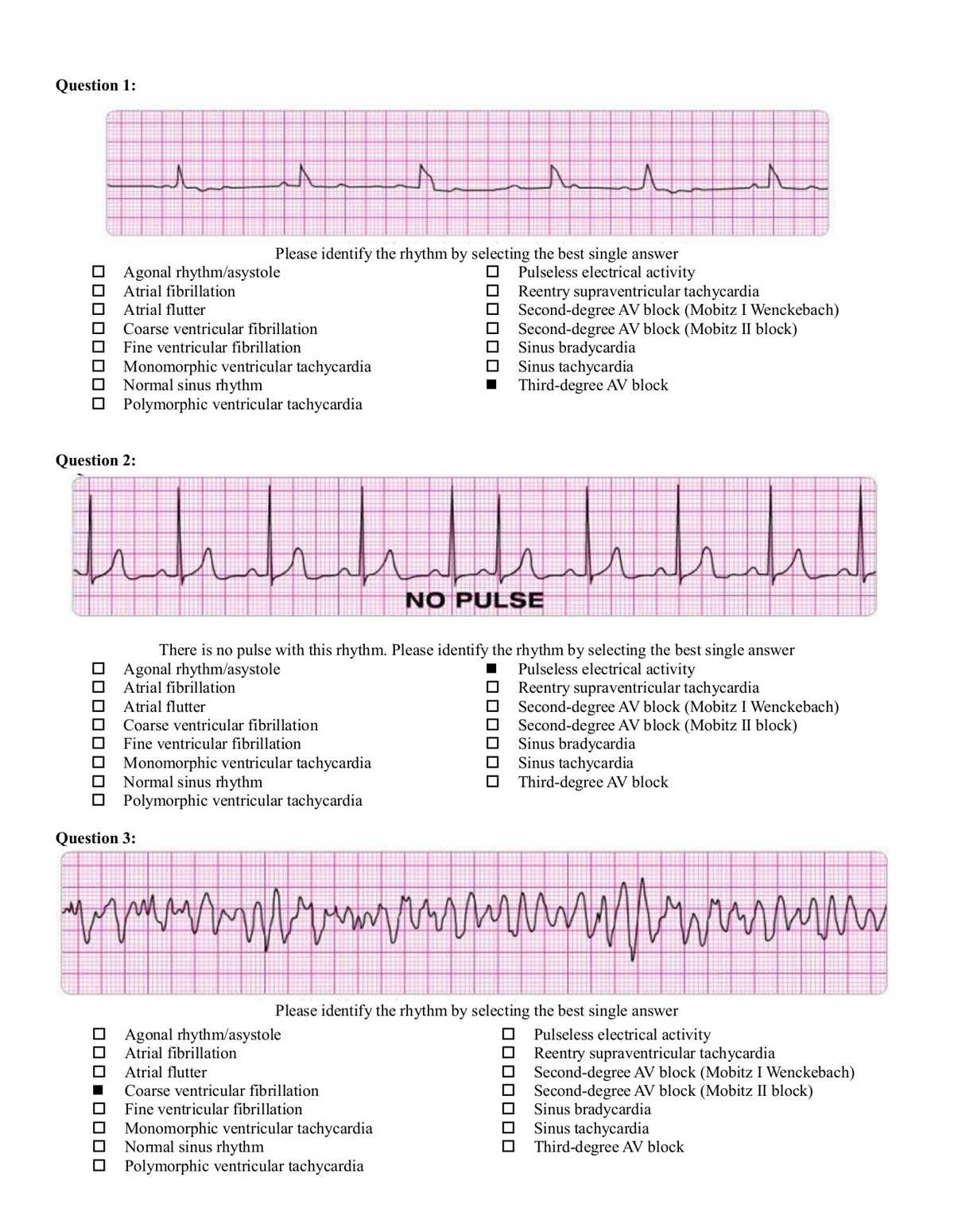
Cardiac arrest management in Advanced Cardiac Life Support (ACLS) is a crucial element of emergency medical care. The primary goal of ACLS in cardiac arrest is to restore and maintain spontaneous circulation in the patient. This is achieved through a systematic approach that encompasses key interventions and algorithms.
One important aspect of ACLS is the early recognition of cardiac arrest. This involves promptly identifying the absence of a palpable pulse and unresponsiveness in the patient. Once cardiac arrest has been confirmed, immediate cardiopulmonary resuscitation (CPR) should be initiated, starting with chest compressions and rescue breaths according to the current guidelines.
ACLS also emphasizes the importance of early defibrillation in the management of cardiac arrest. Rapid defibrillation with an automated external defibrillator (AED) or a manual defibrillator is crucial in cases of cardiac arrest caused by ventricular fibrillation or pulseless ventricular tachycardia. The defibrillation process aims to restore the heart’s normal rhythm and improve overall patient outcomes.
Key interventions in ACLS for cardiac arrest management include:
- High-quality CPR: Compressions and ventilations should be performed correctly to maximize blood flow and oxygenation.
- Advanced airway management: Securing the airway with an endotracheal tube or supraglottic airway device is essential for optimizing oxygenation and ventilation.
- Medication administration: ACLS guidelines provide specific recommendations for the administration of medications, including epinephrine, amiodarone, and vasopressin, based on the underlying rhythm and patient characteristics.
- Post-resuscitation care: After successful resuscitation, a comprehensive approach to post-cardiac arrest care should be implemented, including targeted temperature management, coronary angiography, and early initiation of neuroprotective measures.
Understanding and applying the principles of cardiac arrest management in ACLS is vital for healthcare providers involved in emergency care. By regularly reviewing and practicing these concepts, healthcare professionals can confidently and effectively manage cardiac arrest scenarios, leading to improved patient outcomes.
Mastering Advanced Airway Management Techniques
Advanced airway management in emergency situations is a critical skill that healthcare providers must master. Efficient and effective airway management is essential for maintaining oxygenation, ventilation, and patient stability. By employing advanced techniques, providers can ensure the best possible outcomes for patients in need of airway intervention.
One key aspect of mastering advanced airway management techniques is understanding the indications and contraindications for each approach. Providers must be able to assess quickly and accurately the patient’s condition and determine the most appropriate approach to secure the airway. This may include techniques such as endotracheal intubation, supraglottic airway device insertion, or cricothyrotomy.
Additionally, providers must have a thorough understanding of the equipment used for advanced airway management. This includes familiarity with different types of laryngoscopes, endotracheal tubes, and supraglottic airway devices. Being able to select and use the appropriate equipment for each patient is crucial to ensuring successful airway management.
Furthermore, providers must be proficient in the techniques themselves, including proper placement and verification of tube position, effective suctioning, and timely recognition and management of complications. Regular practice and ongoing training are necessary to maintain and enhance these skills, as advanced airway management techniques may not be utilized frequently in routine clinical practice.
In conclusion, mastering advanced airway management techniques is crucial for healthcare providers in emergency situations. It requires a comprehensive understanding of indications and contraindications, familiarity with equipment, and proficiency in the techniques themselves. By continuously improving these skills, providers can ensure optimal patient outcomes and contribute to saving lives in critical situations.