
A soap physical exam, also known as a comprehensive physical examination, is a systematic and thorough assessment of a patient’s overall health and well-being. It involves a detailed evaluation of the patient’s body systems, including the cardiovascular, respiratory, gastrointestinal, musculoskeletal, and neurological systems, among others.
The soap acronym stands for Subjective, Objective, Assessment, and Plan, which outlines the process that healthcare professionals follow during a physical exam. The subjective component involves gathering information about the patient’s medical history, including any current symptoms or concerns. The objective component involves the physical examination itself, where the healthcare provider assesses the patient’s vital signs, palpates various body parts, listens to the heart and lungs, and performs other necessary tests.
During the soap physical exam, the healthcare provider also evaluates the patient’s overall appearance, mental status, and skin condition. They may also assess specific body systems based on the patient’s age, gender, and any associated risk factors. For example, they may conduct a breast examination in female patients or a prostate exam in male patients. Additionally, the healthcare provider may order laboratory tests or imaging studies to further evaluate any abnormalities or concerns identified during the physical exam.
The soap physical exam is an essential aspect of healthcare, as it allows healthcare providers to detect and monitor medical conditions, identify risk factors, and provide appropriate treatment and care. It serves as a foundation for forming a diagnosis and developing a treatment plan. Through a comprehensive physical examination, healthcare professionals can gain valuable insights into a patient’s health status and work towards promoting their overall well-being.
What Is a SOAP Physical Exam?
A SOAP physical exam, also known as a SOAP note, is a method used by healthcare professionals to document patient encounters. It follows a specific format to ensure comprehensive and organized documentation of a patient’s medical history, physical examination findings, diagnosis, and treatment plan. The SOAP acronym stands for Subjective, Objective, Assessment, and Plan.
Firstly, the subjective component involves gathering information from the patient regarding their symptoms, medical history, and any concerns they may have. This includes demographic details, chief complaints, and a review of systems. The healthcare provider may ask questions about the patient’s current condition, previous illnesses, medications, and allergies.
- Subjective: Gathering information from the patient about their symptoms and medical history.
- Objective: Conducting a physical examination and recording measurable data such as vital signs, laboratory results, and imaging studies.
- Assessment: Analyzing the subjective and objective findings to determine a diagnosis or differential diagnoses.
- Plan: Formulating a treatment plan based on the assessment, which may include medication, referrals, further tests, or follow-up appointments.
Overall, the SOAP physical exam is a systematic approach that enables healthcare professionals to effectively communicate and track a patient’s progress. It promotes standardized documentation and ensures that all relevant information is included, aiding in continuity of care and facilitating interdisciplinary collaboration.
Definition and Purpose
The Soap physical exam, also known as the SOAP note or SOAP documentation, is a method of recording and organizing patient information in a structured format. SOAP stands for Subjective, Objective, Assessment, and Plan, which are the four main components of each entry in a SOAP note.
The purpose of the Soap physical exam is to provide healthcare professionals with a systematic way to document and communicate relevant patient information. It allows for a standardized and concise format that can be easily understood and interpreted by other healthcare providers. The SOAP note is an essential tool for effective communication and collaboration among healthcare team members, ensuring continuity of care and optimal patient outcomes.
The Subjective section of the SOAP note includes the patient’s complaints, symptoms, medical history, and other subjective information reported by the patient or obtained through interviews. This section provides valuable insights into the patient’s perspective and helps in understanding their symptoms and concerns.
The Objective section of the SOAP note includes measurable and observable data gathered during the physical examination, such as vital signs, laboratory results, imaging studies, and physical findings. This section provides objective evidence to support the assessment and diagnosis of the patient.
The Assessment section of the SOAP note includes the healthcare professional’s clinical impressions, diagnosis, and evaluation of the patient’s condition based on the subjective and objective data. This section helps in formulating a comprehensive understanding of the patient’s health status.
The Plan section of the SOAP note includes the healthcare professional’s treatment plan, interventions, prescriptions, referrals, and follow-up recommendations for the patient. This section outlines the steps to be taken to address the patient’s health issues and promote their well-being.
In conclusion, the Soap physical exam is a structured documentation format that enables healthcare professionals to record and communicate patient information effectively. By following the SOAP format, healthcare providers can ensure comprehensive documentation and promote interdisciplinary collaboration for the best possible patient care.
Components of a SOAP Physical Exam

The SOAP physical exam is an important component of a patient’s healthcare assessment. It allows healthcare providers to gather objective information about a patient’s physical condition, which can aid in diagnosis and treatment planning. The physical exam consists of several key components, including:
1. Inspection:
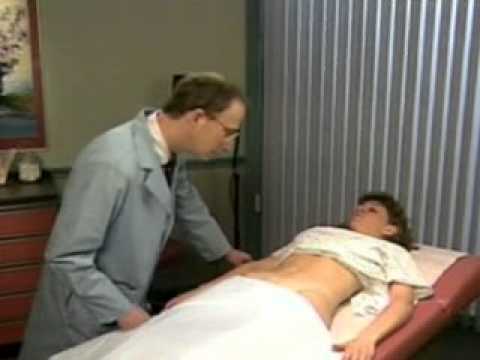
During inspection, the healthcare provider visually examines the patient’s body and specific areas of concern. This may involve observing the skin color, texture, and any abnormalities such as rashes, wounds, or swelling. Inspection can also include assessing the patient’s posture, gait, and overall physical appearance.
2. Palpation:
Palpation involves using the hands to touch and feel specific areas of the patient’s body. Healthcare providers may use gentle pressure to evaluate the texture, temperature, and tenderness of various body parts, such as the abdomen, joints, or lymph nodes. Palpation can help detect abnormalities, such as lumps or enlarged organs.
3. Percussion:
Percussion is a technique where healthcare providers tap specific body areas with their fingers or a special instrument to produce sound. This can help determine the underlying density of the tissue or organ being tapped. Different sounds, such as resonance, dullness, or tympany, can indicate normal or abnormal conditions within the body.
4. Auscultation:
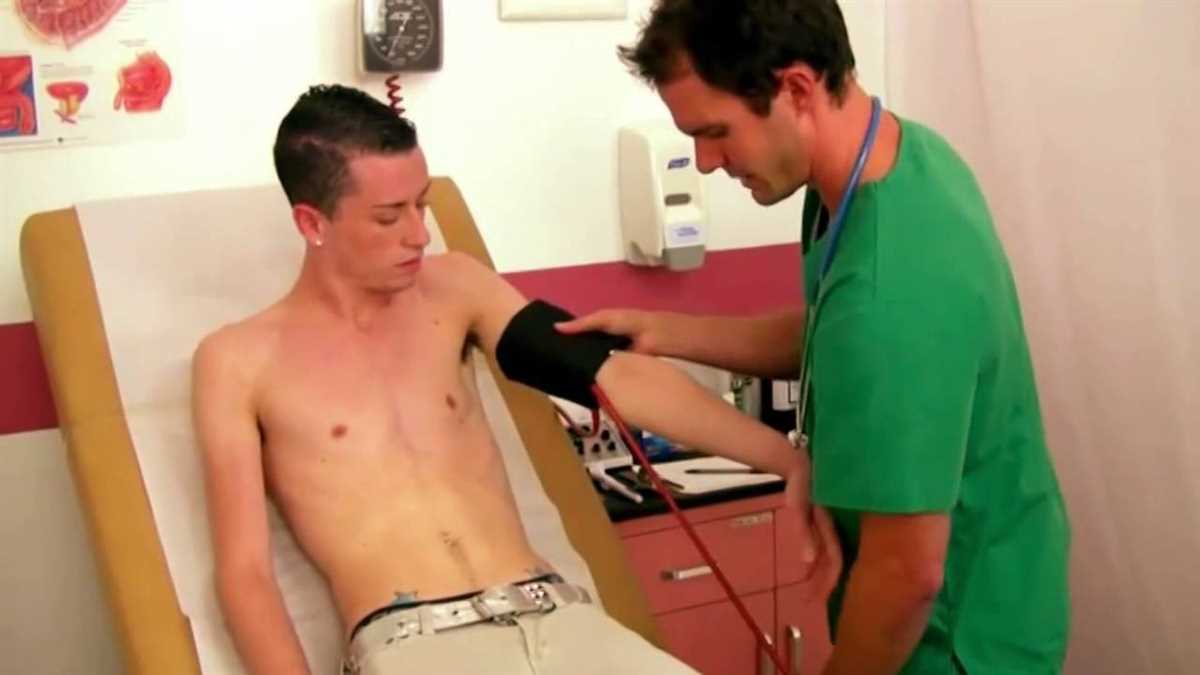
Auscultation involves listening to the sounds produced by the body using a stethoscope. This is commonly done to assess the heart, lungs, and gastrointestinal system. By listening to the heart’s rhythm, lung sounds, or bowel sounds, healthcare providers can gather valuable information about the functioning and potential abnormalities of these organs.
5. Measurements:
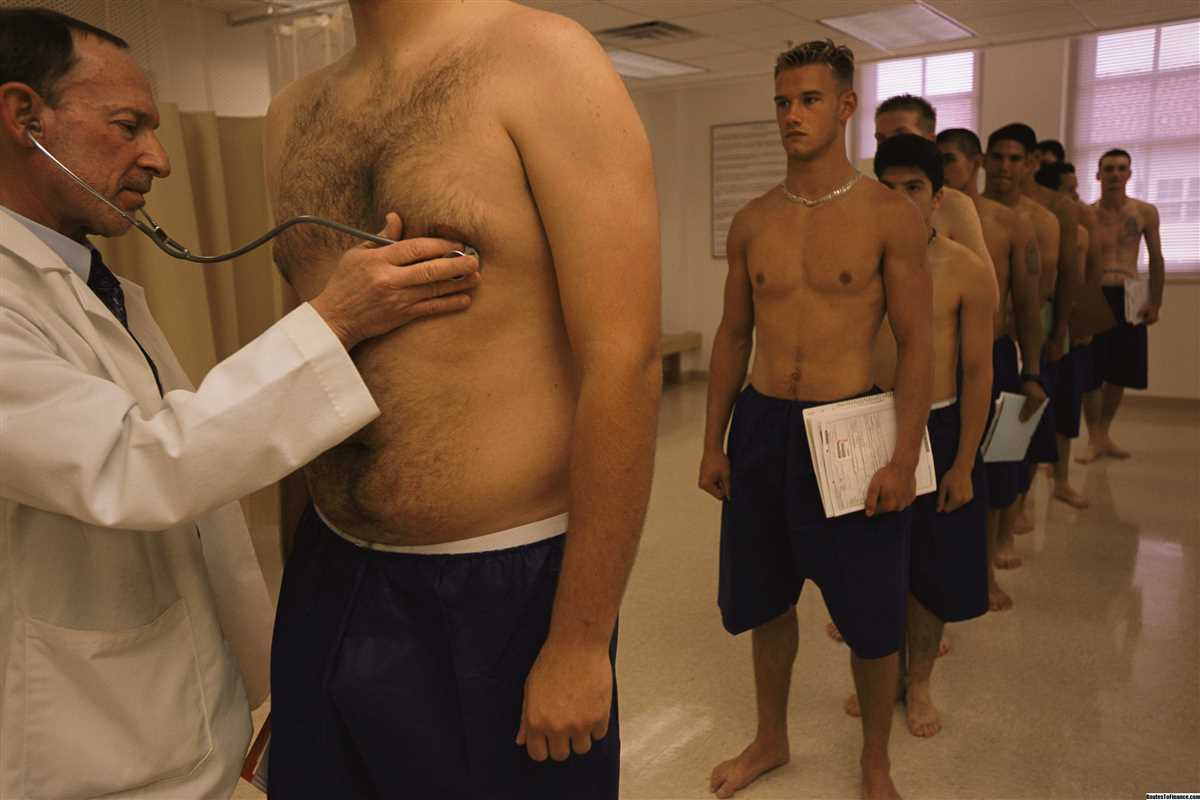
In addition to the physical examination techniques mentioned above, healthcare providers may also take various measurements, such as blood pressure, pulse rate, respiratory rate, and body temperature. These measurements provide quantitative data about a patient’s vital signs, which can help in evaluating their overall health and detecting any abnormalities.
The SOAP physical exam is a comprehensive assessment that combines these components to provide a thorough evaluation of a patient’s physical condition. It allows healthcare providers to gather valuable data and make informed decisions regarding diagnosis, treatment, and ongoing care.
Subjective Assessment
During the subjective assessment phase of the SOAP physical exam, the healthcare provider gathers information about the patient’s symptoms, medical history, and current complaints. This helps to establish a comprehensive understanding of the patient’s condition and guides further examination and treatment.
The healthcare provider begins by asking the patient open-ended questions to allow them to freely discuss their concerns and provide relevant information. This may include questions about the onset and duration of symptoms, any associated pain or discomfort, and any exacerbating or relieving factors. The provider also inquires about the patient’s medical history, including past illnesses, surgeries, and any current medications or allergies.
Strong communication skills are essential during the subjective assessment as they help establish rapport and trust with the patient. Active listening allows the provider to gather detailed information, while empathy and non-judgmental behavior create a safe environment for the patient to share their experiences. Both the provider and patient should engage in open dialogue throughout the assessment to ensure all relevant information is captured.
- Sample Questions:
- Can you describe your symptoms in detail?
- When did the symptoms first start?
- Have you noticed any patterns or triggers for your symptoms?
- Do you have any past medical conditions or surgeries?
- Are you currently taking any medications or supplements?
The subjective assessment is a critical part of the SOAP physical exam as it provides valuable insight into the patient’s condition. By gathering and analyzing this information, the healthcare provider can develop an appropriate plan of care and address the patient’s specific needs. It also helps in forming a strong patient-provider relationship based on trust, communication, and mutual respect.
Objective Assessment
In the objective assessment part of the SOAP physical exam, the healthcare provider records the findings from the physical examination and any diagnostic tests performed. This section contains specific and measurable information about the patient’s condition.
During the physical examination, the healthcare provider examines the patient’s body systems and documents any abnormal findings. This may include measuring vital signs such as blood pressure, heart rate, and respiratory rate. They may also assess the patient’s general appearance, skin condition, and neurological function.
The healthcare provider may also order diagnostic tests to further investigate the patient’s condition. These tests may include laboratory tests, imaging studies, or special procedures. The results of these tests are recorded in the objective assessment section of the SOAP note.
To ensure accuracy and consistency, the objective assessment should be recorded in a clear and concise manner. Measurements should be documented, and abnormal findings should be described in detail. This section provides a factual basis for the patient’s diagnosis and treatment plan.
The objective assessment is an important part of the SOAP physical exam as it provides an objective and measurable record of the patient’s condition. It allows other healthcare providers to review the patient’s case and make informed decisions about their care.
Assessment
During the physical examination, the healthcare provider assesses various aspects of the patient’s health. This includes evaluating the patient’s overall appearance, vital signs, and general mental status. The provider may observe the patient’s posture, level of distress, and any obvious signs of discomfort or pain. They will also measure the patient’s blood pressure, heart rate, respiratory rate, and temperature, which helps determine the patient’s baseline physiological functions.
The healthcare provider will perform a thorough examination of the patient’s body systems, starting with the head and neck and moving down to the extremities. They will assess the patient’s eyes, ears, nose, throat, and lymph nodes, looking for any abnormalities or signs of infection. The provider will also listen to the patient’s heart and lungs using a stethoscope to check for any abnormal sounds or murmurs.
The provider will continue the assessment by examining the patient’s abdomen, assessing for any tenderness, masses, or abnormal organ enlargement. They will also palpate the patient’s peripheral pulses to check for any abnormalities in circulation. The provider may perform additional tests, such as percussion or auscultation, to further evaluate specific body systems. Overall, the goal of the assessment is to gather objective information about the patient’s health status and identify any potential issues that may require further investigation or treatment.
Plan
Based on the findings from the SOAP physical exam, the following plan has been established for the patient:
- Treatment: The patient will be prescribed a course of antibiotics to treat the underlying infection.
- Monitoring: The patient will be closely monitored for any signs of improvement or worsening of symptoms.
- Follow-up: A follow-up appointment will be scheduled in one week to assess the patient’s progress.
- Home care instructions: The patient will be provided with detailed instructions on wound care, including proper cleaning and dressing techniques to prevent infection.
In addition to the above plan, the patient will also be advised to rest and avoid any strenuous activities until fully recovered. It is important for the patient to adhere to the prescribed medication regimen and attend all scheduled follow-up appointments for a successful recovery.
Importance of a SOAP Physical Exam
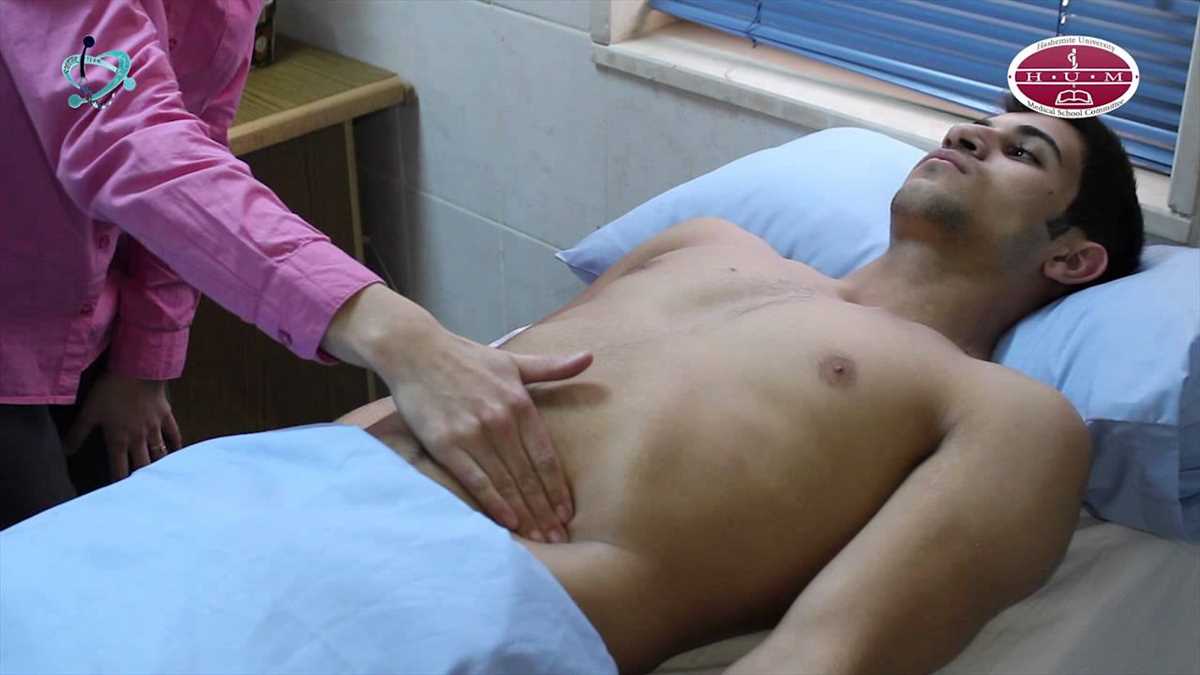
A SOAP physical exam is a vital component of a patient’s medical assessment. This type of examination is structured and comprehensive, ensuring that no aspect of the patient’s health is overlooked. SOAP stands for Subjective, Objective, Assessment, and Plan, and it serves as a framework for organizing the information gathered during the examination.
Subjective: The subjective part of the SOAP physical exam involves obtaining relevant information directly from the patient. This includes their medical history, current symptoms, and any concerns they may have. By gathering this subjective data, healthcare providers gain valuable insights that help inform the rest of the examination and subsequent diagnosis.
Objective: The objective part of the SOAP physical exam includes the collection and analysis of measurable data. This can include vital signs such as blood pressure and heart rate, as well as the physical examination itself. During the physical examination, healthcare providers assess various systems of the body, such as the respiratory, cardiovascular, and musculoskeletal systems.
Assessment: Once the subjective and objective data have been collected, healthcare providers analyze and interpret the information to form an assessment of the patient’s health. This assessment can include the identification of any abnormalities or potential underlying conditions. By having a thorough understanding of the patient’s health status, healthcare providers can provide appropriate treatment and interventions.
Plan: The final step of the SOAP physical exam involves developing a plan for further investigation, treatment, and ongoing care. This can include ordering additional tests or referrals to specialists, prescribing medications, or recommending lifestyle modifications. The plan is tailored to the individual patient and their specific needs based on the findings from the subjective and objective assessment.
In conclusion, the SOAP physical exam is of utmost importance in healthcare as it allows for a systematic and comprehensive evaluation of a patient’s health. By following the SOAP framework, healthcare providers are able to gather and analyze all necessary information to make an accurate assessment and develop an appropriate plan for the patient’s care.