The Health Insurance Portability and Accountability Act (HIPAA) is a federal law that protects the privacy and security of individuals’ health information. Compliance with HIPAA is essential for any healthcare organization or professional to ensure patient confidentiality and maintain trust. To assess knowledge and understanding of HIPAA regulations, individuals may take a HIPAA privacy test. This article provides answers to common questions and scenarios that may appear in a HIPAA privacy test.
One question that may arise in a HIPAA privacy test is regarding the purpose of the Privacy Rule. The Privacy Rule establishes national standards to protect individuals’ medical records and other personal health information. It grants patients certain rights over their health information and sets boundaries on how healthcare providers and entities can use and disclose this information. The Privacy Rule aims to strike a balance between protecting individuals’ privacy and facilitating the flow of necessary information for healthcare and related purposes.
Another question that may be asked in a HIPAA privacy test is related to permissible disclosures of protected health information (PHI) without patient authorization. Under HIPAA, healthcare providers can disclose PHI without patient authorization in certain situations, such as for treatment, payment, and healthcare operations. However, it is important for healthcare professionals to always consider the minimum necessary principle and limit disclosures to the information that is necessary for the intended purpose.
Additionally, a HIPAA privacy test may include scenarios about breaches of privacy and security. In the event of a breach, HIPAA requires covered entities to notify affected individuals, the Department of Health and Human Services, and, in certain cases, the media. Timely response and appropriate actions must be taken to mitigate the breach and prevent further unauthorized access to individuals’ health information. Training and awareness programs for healthcare employees are crucial to prevent breaches and ensure compliance with HIPAA regulations.
HIPAA Privacy Test Answers
Understanding and adhering to HIPAA (Health Insurance Portability and Accountability Act) regulations is crucial for healthcare providers in order to protect patient privacy and maintain confidentiality. HIPAA Privacy Test is designed to assess the knowledge and understanding of these regulations. Here are some test answers for common questions:
1. What is considered Protected Health Information (PHI)?
Protected Health Information includes any individually identifiable health information that is created, received, or maintained by a covered entity (healthcare provider). This can include medical records, billing information, health insurance details, and any other information related to an individual’s past, present, or future medical condition.
2. What are the main requirements for HIPAA compliance?
- Ensure the confidentiality, integrity, and availability of PHI
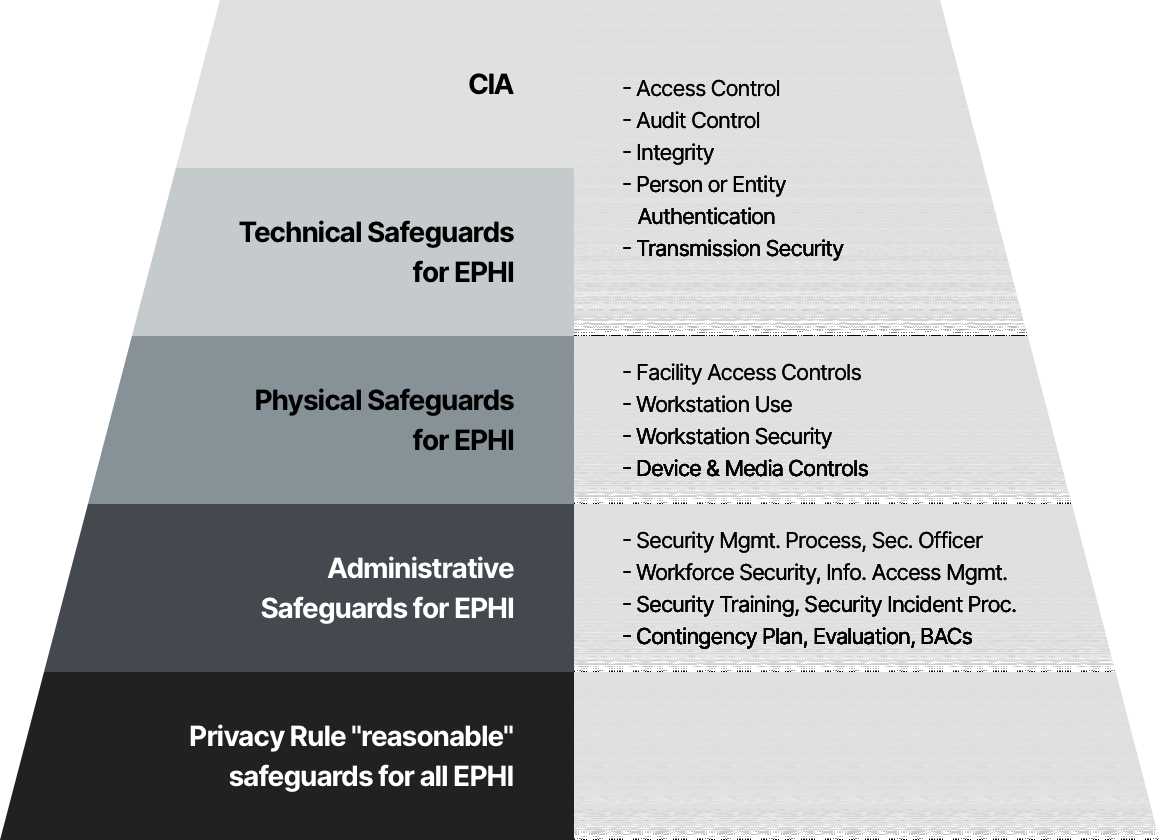
- Implement administrative, physical, and technical safeguards to protect PHI
- Develop and implement policies and procedures for HIPAA compliance
- Train employees on HIPAA regulations and the proper handling of PHI
- Conduct regular risk assessments to identify potential vulnerabilities
3. How should healthcare providers handle a breach of PHI?
In the event of a breach of PHI, healthcare providers must follow certain procedures to mitigate the impact and comply with HIPAA regulations. These steps include:
- Assess the nature and extent of the breach
- Notify affected individuals in a timely manner
- Report the breach to the appropriate authorities, such as the Office for Civil Rights (OCR)
- Implement measures to prevent future breaches
4. Can PHI be disclosed without patient consent?
Under HIPAA, PHI can be disclosed without patient consent in certain situations, such as for treatment, payment, and healthcare operations. However, healthcare providers must still follow the minimum necessary rule, which means disclosing only the minimum amount of PHI necessary for the specific purpose.
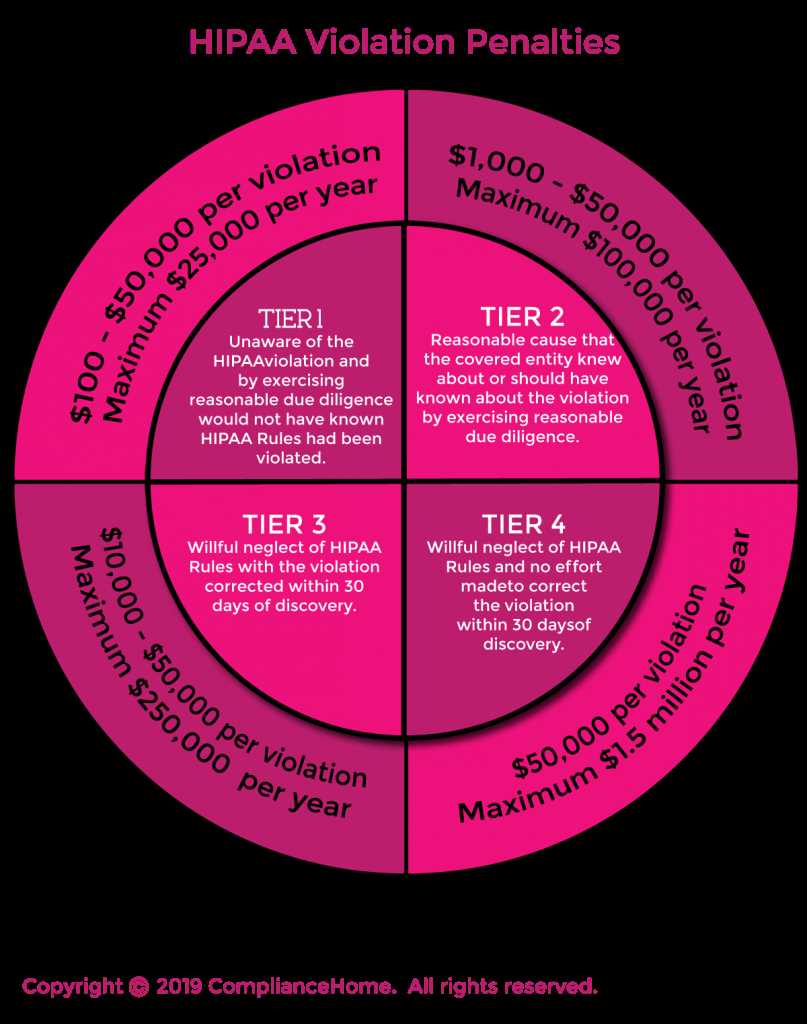
5. What are the penalties for HIPAA violations?
The penalties for HIPAA violations can vary depending on the severity of the violation. They can range from financial penalties, such as fines, to criminal charges. The Office for Civil Rights (OCR) is responsible for enforcing HIPAA regulations and imposing penalties.
Staying up to date with HIPAA Privacy regulations is essential to ensure patient privacy and maintain compliance. By familiarizing themselves with these answers, healthcare providers can better protect patient information and avoid potential violations.
Understanding HIPAA Privacy Rules
The Health Insurance Portability and Accountability Act (HIPAA) includes privacy rules that are designed to protect individuals’ medical information. These rules establish standards for how healthcare providers and other covered entities handle and maintain sensitive patient data.
Under HIPAA privacy rules, covered entities are required to keep patients’ medical information secure and confidential. This includes not only electronic records, but also paper documents and other forms of physical records. Covered entities must implement safeguards to prevent unauthorized access to patient information, such as secure storage, passwords, and encryption.
Additionally, HIPAA privacy rules give individuals the right to access and control their own medical information. This means that patients have the right to request copies of their medical records, make corrections to any inaccurate information, and set restrictions on who can access their information.
To ensure compliance with HIPAA privacy rules, covered entities must train their employees on privacy policies and procedures, maintain strict disciplinary measures for any violations, and regularly conduct risk assessments to identify and address potential vulnerabilities in their data security systems.
Overall, understanding HIPAA privacy rules is essential for healthcare providers and other covered entities to ensure the protection of patient information and maintain compliance with legal requirements. By implementing proper safeguards and providing individuals with control over their own medical information, organizations can uphold the privacy and confidentiality of patients’ sensitive data.
HIPAA Privacy Test Overview

The Health Insurance Portability and Accountability Act (HIPAA) Privacy Test is a comprehensive examination that assesses an individual’s understanding of privacy regulations and guidelines prescribed by HIPAA. HIPAA is a federal law implemented to safeguard the privacy and security of individuals’ protected health information (PHI) and ensure its confidentiality. This test is designed to evaluate the knowledge and comprehension of healthcare providers, employees, and individuals working with PHI to ensure compliance with HIPAA requirements.
The HIPAA Privacy Test covers various aspects related to privacy and security measures that need to be implemented to protect PHI. The test includes questions about the types of information considered as PHI, the individuals and organizations covered by HIPAA regulations, the rights of individuals regarding their PHI, and the responsibilities and obligations of healthcare providers and employees. It also assesses knowledge on HIPAA administrative safeguards, physical safeguards, technical safeguards, and breach notification requirements.
Topics Covered in the HIPAA Privacy Test:

- Definition and classification of protected health information (PHI)
- Covered entities and business associates
- Individual rights under HIPAA
- Required safeguards for protecting PHI
- HIPAA breach notification requirements
- Penalties and enforcement actions for non-compliance
The HIPAA Privacy Test is an essential tool to ensure compliance with HIPAA regulations and protect individuals’ privacy rights. By successfully completing this test, individuals and organizations can demonstrate their understanding of HIPAA requirements and their commitment to maintaining the privacy and security of PHI. It serves as a benchmark to assess the level of knowledge and identify areas that may require further training or improvement.
Common HIPAA Violations
HIPAA (Health Insurance Portability and Accountability Act) violations can occur in various healthcare settings and can result in significant penalties and fines. It is crucial for healthcare professionals and organizations to be aware of these violations and take measures to prevent them. Here are some common HIPAA violations:
1. Unauthorized access to patient information
One of the most common HIPAA violations is unauthorized access to patient information. This can occur when healthcare employees access patient records without a legitimate reason or without proper authorization. It is essential for healthcare organizations to implement strict access controls and train their staff on the importance of patient privacy.
2. Improper disposal of patient records
Another common violation is the improper disposal of patient records. HIPAA regulations require healthcare organizations to dispose of patient records in a way that ensures their confidentiality. This includes shredding or securely disposing of physical records and using secure methods to delete or destroy electronic records.
3. Lack of encryption or data security
Failure to implement proper encryption or data security measures is another common HIPAA violation. Healthcare organizations must take steps to protect patient information from unauthorized access, including encrypting electronic medical records and using secure communication channels for transmitting sensitive data.
4. Failure to provide patients with access to their own records
HIPAA grants patients the right to access their own medical records. Failure to provide patients with their records within a reasonable time frame can be a violation. Healthcare organizations must have processes in place to handle patient requests for access to their records and ensure compliance with HIPAA requirements.
5. Breach notifications
Under HIPAA, healthcare organizations must notify affected individuals in the event of a breach of their protected health information. Failure to properly notify patients or delayed notifications can result in violations. Healthcare organizations should have a breach notification process in place to promptly inform patients and take appropriate actions to mitigate the breach.
Answers to HIPAA Privacy Test Questions

Below are the answers to some common questions that may arise during a HIPAA privacy test:
1. What does HIPAA stand for?
HIPAA stands for the Health Insurance Portability and Accountability Act.
2. What is the primary goal of HIPAA?
The primary goal of HIPAA is to protect the privacy and security of an individual’s health information.
3. Who is required to comply with HIPAA regulations?
All covered entities, including healthcare providers, health plans, and healthcare clearinghouses, are required to comply with HIPAA regulations.
4. What is protected health information (PHI)?
PHI refers to any individually identifiable health information that is created, received, maintained, or transmitted by a covered entity in any form or medium.
5. What are the key privacy requirements under HIPAA?
- Obtaining patient consent for the use and disclosure of PHI
- Maintaining appropriate safeguards to protect PHI
- Limited use and disclosure of PHI
- Providing individuals with rights to their PHI
- Notifying individuals about privacy practices
6. What is a HIPAA breach?
A HIPAA breach is any unauthorized acquisition, access, use, or disclosure of PHI that compromises the privacy or security of the information.
7. What are the penalties for HIPAA violations?
The penalties for HIPAA violations can range from monetary fines to criminal charges, depending on the severity of the violation. The fines can be as high as $50,000 per violation, with an annual maximum of $1.5 million.
8. What steps should be taken in the event of a potential HIPAA breach?
If a potential HIPAA breach is identified, the covered entity should immediately conduct a risk assessment to determine the likelihood of harm to individuals. If required, individuals affected by the breach should be notified, and appropriate corrective actions should be taken to prevent future breaches.
9. How can covered entities ensure compliance with HIPAA?
Covered entities can ensure compliance with HIPAA by implementing policies and procedures that address the privacy and security requirements, providing training to employees, regularly assessing internal controls, and conducting periodic audits to identify areas of improvement.
10. How long should covered entities retain PHI?
Covered entities are required to retain PHI for a minimum of six years from the date of creation or the date when it was last in effect, whichever is later. However, state laws may impose longer retention periods.
Overall, understanding HIPAA regulations and maintaining compliance is essential for protecting the privacy and security of individuals’ health information.
The Importance of HIPAA Compliance

HIPAA, or the Health Insurance Portability and Accountability Act, is a crucial piece of legislation in the healthcare industry. It was enacted in 1996 to protect the privacy and security of patients’ health information and establish standards for healthcare organizations to follow. HIPAA compliance is of utmost importance for a number of reasons.
Protecting Patient Privacy: One of the primary goals of HIPAA is to safeguard the privacy of patients’ health information. This includes any individually identifiable information such as medical history, diagnosis, treatment plans, and personal identifiers. By enforcing strict guidelines on how healthcare organizations handle, store, and share this information, HIPAA ensures that patients’ privacy rights are respected and protected.
Preventing Data Breaches: With advancements in technology, healthcare organizations are at an increased risk of data breaches and cyberattacks. HIPAA compliance helps mitigate these risks by requiring organizations to implement security measures, such as encryption and firewalls, to protect patient data. It also mandates regular risk assessments and audits to identify and address any vulnerabilities in the system.
Avoiding Legal Consequences and Penalties: Non-compliance with HIPAA can result in severe legal consequences and penalties for healthcare organizations. These can include fines ranging from thousands to millions of dollars, reputational damage, loss of business, and even criminal charges. By ensuring HIPAA compliance, organizations can avoid these adverse consequences and protect their reputation.
Building Trust with Patients: HIPAA compliance plays a vital role in building trust with patients. When patients know that their health information is being handled in a secure and confidential manner, they are more likely to feel comfortable sharing their sensitive information with healthcare providers. Trust is crucial in maintaining a strong patient-provider relationship and ensuring quality healthcare delivery.
In conclusion, HIPAA compliance is essential for protecting patients’ privacy, preventing data breaches, avoiding legal consequences, and building trust with patients. Healthcare organizations must prioritize HIPAA compliance to uphold the integrity and confidentiality of patients’ health information.